Hyperthermia and Immunotherapy[1]:
The Gorter Model
*Robert Gorter, MD, PhD, and **Erik Peper, PhD
“I would cure all diseases if I only could produce fever.”
Parmenides, Greek physician, 510 BC
Fever turns out to be one of the missing links in understanding the cause and the therapy of cancer. A growing body of research suggests that most cancer patients have a lower core temperature and cannot mount a fever, and thus are unable to activate their immune system. In the clinical setting, these patients report having never experienced a fever. The research provides strong evidence for this correlation.
Cancer, Fever, and Circadian Rhythm
An extensive body of research suggests that many cancer patients have a lower core body temperature—on average 0.8oF/0.5oC lower than the average person. There may also be an inconsistent pattern in the rhythm of their temperature over a 24-hour period (as shown in Figure 1).
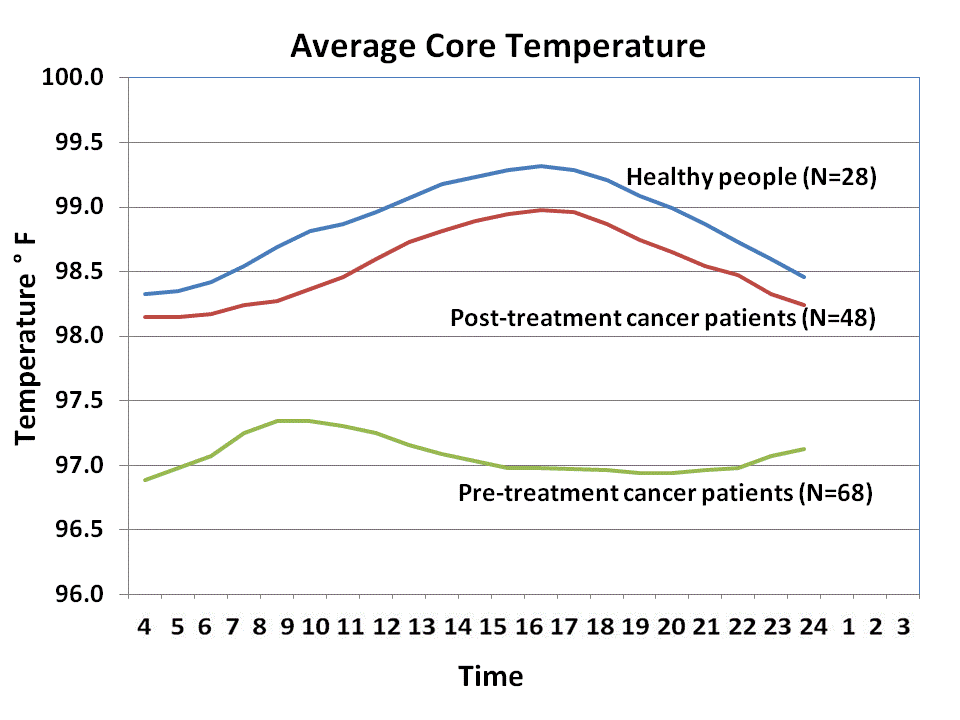
Figure 1. Average rectal core temperature over 24 hours for healthy adult controls compared with the temperature of cancer patients before and after treatment. Data: Gorter, Medical Center Cologne. Reproduced by permission from Gorter, R. and Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment. Berkeley: North Atlantic Books
Dr. Gorter: In our clinical experience at the Medical Center Cologne (MCC) in Germany and in other countries, these patients typically report that they often feel chilly or cold, with cold hands and feet, and that this has been a frequent pattern for the past several years. Documenting their actual temperature, we find that their natural circadian rhythm for temperature is absent or disrupted.
Cancer patients also report that they were seldom ill before they developed cancer. They may have experienced brief bouts of a sore throat, a cold, or a cough, but these illnesses were almost never accompanied by a fever. These cancer patients, like most people in industrial societies, habitually use aspirin, acetaminophen, or antibiotics at the first sign of a fever.

Gorter Model / Medical Center Cologne (MCC) in Cologne, Germany (2000-2018)
Fever as the Source of Immune Activation
When body temperature reaches 101.3° F (38.5° C), typically the immune system shifts into a state of intensive activity. At this temperature, immune factors, in the bloodstream increase two-fold or greater, and in some cases as high as ten-fold, triggering activation of immune defenses throughout the body. Numerous studies have reported higher levels of messenger chemicals, white blood cells, and immune scavengers in response to fever, including:
- Heat shock proteins
- Interleukins and other cytokines
- Human growth hormone
- Antigen-presenting dendritic cellsxxii
- Lymphocytes such as NK cellsxxv and T-cellsxxii
- Macrophages and other phagocytes
- Antibodies
- Increased numbers of circulating and activated stem cells
In vitro research at the University of Vienna found a 10-fold increase in monocytes when blood was heated to 102.2 F (39 C). These researchers confirmed that one of the mechanisms which promote this increase was higher levels of heat shock proteins in the bloodstream.[2]
NIH (National Institute of Health) on Fever as the Missing Link in Cancer
One of the most insightful looks at the role of fever in healing has come from a research team from the National Institutes of Health. The researchers performed an in-depth review of the medical literature on cancer risk. They reported that risk appears to be increased in individuals who have a history of fewer infections. They noted “an inverse correlation between the incidence of infectious diseases and cancer risk. In sum, people who have not experienced common childhood illness and fever apparently have a greater risk of cancer.
Averting fever with the frequent use of aspirin, acetaminophen, or antibiotics may actually impair immune function. The NIH team concluded that “the occurrence of fever in childhood or adulthood may protect against the later onset of malignant disease.”[3],[4] Researchers also pointed out that “spontaneous remissions are often preceded by feverish infections.” iv,v Their final report includes hundreds of references from the medical and research literature.iv
A Century of Research on Fever and Cancer
A number of researchers have tracked this issue in large clinical trials over the past 100 years, starting with published reports in 1854 that many cancer patients have a “remarkable disease-free history.”[5] Several later studies confirmed this, reporting that people who developed cancer were rarely ill before their disease.

William Bradley Coley (1862-1936) was an American orthopedic surgeon and oncologist. With his development of hyperthermia (fever) in cancer treatment, he is considered the father of modern Cancer Immunotherapy.
Studies on the importance of fever as an immune defense against cancer were published in the medical literature in 1854, 1910, 1934, and 1936, each study involved hundreds of patients. Researchers consistently found increased cancer risk for patients who had no history of infectious illness or fever.[6] The majority of more recent studies have corroborated these findings.
- German research published in 1983 found that cancer risk more than doubled in patients who had not experienced major infectious diseases (2.6 times greater risk). Cancer risk was almost 6-fold higher in patients who had never experienced the common cold (5.7 odds ratio), and there was a 15-fold increase for those who had never experienced fever (15.1 odds ratio).[7]
- A study of skin cancer patients, published in Melanoma Research in 1992 reviewed the medical histories of 500 comparable patients, with and without cancer. Researchers found that the patients who had experienced infections accompanied by fever had a much lower incidence of malignant melanoma.[8]
- Research published in the journal Cancer in 1992 evaluated the medical histories of more than 200 patients with brain tumors, who were compared with over 400 similar non-cancerous patients. Those who had experienced infections and colds had a 70% lower risk of cancer.[9]
- In a randomized control trial of 572 critically ill patients, published in 2005 in Surgical Infections, 82 patients with high fever were further study evaluated. Half these patients received aggressive fever suppression and the other half were advised to assume watchful waiting. There were seven deaths in the aggressive group and only one death occurred in the watchful waiting group.[10]
- In a recent study of 400 hospitalized pneumonia patients, the British Medical Journal reported that the more feverish the patient on admission, the better their chance of 30-day survival.[11] Of patients admitted with a low core temperature (<96.8ºF or 36ºC) 34% died; among those with higher than normal core temperature (>100.4ºF or 38ºC), only 17% died within 30 days of admission.
These studies and many others demonstrate that fever suppression tends to inhibit the immune response and healing. The research also suggests that when fever is tolerated by the patient through careful watchful monitoring, frequently improves outcome.
Conditioning of the Fever Response
Surprisingly, the immune system can be trained to turn on or off in response to repeated cues, for example in reaction to certain medications. This trained or “conditioned” response was demonstrated in the work of Dr. Robert Ader and colleagues, published over a period of 25 years.[12],[13],[14],[15] Researchers found that the immune system could actually be deactivated through “classical conditioning.”
Applying this concept to the use of fever suppressing medications with children, the implication is that over time the fever response can be permanently inactivated by the frequent use of these medications. From that point on, whenever the child develops a fever, the fever process is aborted. With frequent use of fever suppressants in childhood, the immune system may never become fully activated and mature. The immune system is prevented opportunities for a “workout” and becomes less and less adept, leaving the body more vulnerable.
Without an all-out effort by the immune system to completely wipe out an infection, bacterial and viral infections can linger and become chronic. The association of chronic infection with cancer is well documented for conditions that include human papillomavirus and cervical cancer, hepatitis and liver cancer, and H. pylori bacteria and gastric cancer. These factors appear to set the stage for the development of cancer.
HISTORY OF FEVER THERAPY
Fever and heat therapy have been recognized for their beneficial effects on health since antiquity. Ancient Greek medicine, Roman sulfur hot baths, Finnish saunas, European and American spa treatment, Japanese hot tubs, Native American Indian sweat lodges, and therapeutic hot springs worldwide are examples of simple forms of heat therapy as a means of cleansing and healing.
Limitations of traditional approaches. We know from systematic studies in the literature that traditional methods such as saunas, mineral baths, and Jacuzzi do not significantly increase core temperature nor do they achieve temperatures that correspond to internally induced fever. Consequently, a more innovative approach is necessary to raise the body to a therapeutic fever range. This article will discuss contemporary innovations in hyperthermia, as applied in the treatment of cancer.
A study at the Medical University of Hannover, Germany found that when body temperature was raised via warm baths, gradually heated to 42 C (approx 107 F), core temperature actually increased less than one degree Fahrenheit (or 0.4 C) above normal. xxi Body temperature alone does not automatically induce the immune response, demonstrated in a study in Hamburg, Germany. The temperature of cancer patients was increased with hyperthermia and compared with that of healthy volunteers who took part in strenuous physical exercise to raise their temperatures. Although participants in both groups experienced elevated temperatures, immune function increased in the cancer patients, but not in the healthy volunteers. Elevated immune factors in cancer patients included human growth hormone and the induction of natural killer cells and T-cells. xix
Fever: foe or friend? In our culture, there is a pervasive fear of fever, a tendency to see fever as the cause of illness, rather than the body’s natural mechanism for healing. While fever racks the patient, the mother, father, friend, or caretaker stands by feeling powerless. No wonder it is a temptation to quickly reach for medication such as aspirin or Tylenol at the first sign of a fever. Medicine represents hope and recovery. Giving medication implies a cure. (And so does the advertising. The message is: If you can just reduce the fever, the disease will go away.)
Ironically, the fear of fever is misplaced. Unless the fever is too high (104 °F/40.0 °C or above) or persists for weeks at a time, no harm occurs. In fact, fever is the natural response of all mammals to infection or illness. Research has made it clear that fever is not the enemy; it is the friend of healing. This scientific rationale, supported by thousands of research studies, provides the basis for hyperthermia treatment at the Medical Center Cologne and other medical centers in Europe and worldwide.
MEDICAL HYPERTHERMIA
Dr. Gorter: Induced fever or hyperthermia has been studied in hundreds of cancer clinical trials and discussed in thousands of peer-reviewed articles. Research on hyperthermia also referred to as “fever-range total-body hyperthermia” or “moderate whole-body hyperthermia”, has been performed in medical schools and research centers since the 1980s. These studies have been conducted primarily in the U.S., Germany, and Japan. American research has been conducted in FDA-approved studies at the Mayo Clinic, University of Pennsylvania, University of Texas, and Duke. The medical literature reflects a global dialogue between researchers that has systematically defined effective hyperthermia.
The majority of the research has been performed at academic medical and research centers throughout Germany. At the Medical Center Cologne, located in a large teaching hospital in Cologne, Germany, hyperthermia protocol development has been ongoing for the past 25 years under the direction of Robert Gorter, MD, PhD. To reactivate immune function in cancer patients, the Gorter Model uses a controlled fever process in which the entire body is gradually heated through infra-red light to a moderate fever temperature between approximately 101°F and 103o F (38.5° C and 39.5o C) under carefully monitored conditions. These treatments engage the patient’s immune system replicating the natural process of fever, comparable to immune activation in response to an acute infection.
Localized heat treatment is another therapeutic used in the Gorter Model in which a specific area of the body (often a tumor site) is selectively heat. This form of treatment described as “regional hyperthermia” increases the temperature in the targeted malignant cells intra-cellular to 42° C (107.6° F) causing higher levels of intra-cellular lactic acid production, which leads to cell death (necrosis). Localized high temperatures and the resulting death of cancerous cells simultaneously activate the immune system. Surrounding healthy cells are unaffected. Therefore, also patients with primary or secondary cancer can undergo very safely this form of local hyperthermia as brain cells are not affected by this method: only cancer cells are forced to increase their intra-cellular temperature. At the Medical Center Cologne and other associated clinics, this approach is used in approximately 99% of patients.
DEVELOPMENT OF THE GORTER MODEL
The Medical Center Cologne was founded by Robert Gorter, MD, PhD, and has been under his direction for the past 20 years. The Center is dedicated to the treatment of cancer using immune-supportive therapies. He developed this program based on his clinical experience as program director in the field of AIDS research and 50 years in clinical oncology, as well as his personal experiences as a cancer survivor himself.
Dr. Gorter earned his medical degree at the University of Amsterdam Medical School in the Netherlands. He subsequently opened a private practice and health center in the heart of Amsterdam, but a few weeks later was diagnosed with far-advanced stage IV testicular cancer (Germ-Cell Carcinoma)—at that time described as “teratocarcinoma,” a type of cancer currently defined as “germ cell carcinoma.” He was able to recover successfully through non-toxic treatment, without the use of chemotherapy, radiation or surgery. His treatment consisted solely of hyperthermia and injections of a known oncologic botanical, the European mistletoe (Viscum album). This experience has motivated him to explore new, non-toxic approaches to cancer therapy and has inspired his lifelong work as a researcher and clinician in the area of integrative (Translational) cancer oncology.
His exploration of immunotherapy deepened with his appointment as physician and researcher on AIDS at San Francisco General Hospital in the world-renowned Ward 86 in the 1980s When Ward 86 became part of the UCSF AIDS program, Dr. Gorter became medical director of the Department of AIDS Epidemiology and Biostatistics at UCSF and led that department for four years. Much of what we know today about the progression of HIV infection into AIDS comes from the seminal research on this initial cohort of patients whose progress was tracked in long-term follow-up studies at UCSF. Dr. Gorter was intrigued by the fact that a few of the patients with HIV infection never progressed to AIDS or AIDS-Related Complex (ARC), patients described as “long-term, non-progressors.”
This work, conducted at the beginning of the AIDS epidemic in the U.S. and E.U., provided Dr. Gorter the opportunity to be involved in the research and clinical care that first defined the complex elements of the human immune system. These studies from UCSF Medical Center have resulted in the most extensive knowledge base on immunity in HIV infection in our time. Dr. Gorter noticed that most illnesses leading to the death of HIV-infected patients were malignancies. Thus, the decay of the immune system caused by HIV seemed to be correlated with the increase of various forms of cancer.
A decade later, when Dr. Gorter shifted the focus of his work to cancer treatment, he began developing treatment protocol based on the principles of intensive and targeted immune restoration learned in the “war on AIDS.” Dr. Gorter has spent more than two decades establishing and refining the effective methodology for immune therapy. He has pioneered the integrated use of hyperthermia. In addition, he has worked extensively on protocol development, for dendritic cell vaccination, which is used in combination with mistletoe botanicals, antioxidant treatment, and other immune restorative agents. Mistletoe, for example, is known to balance biological rhythms in the body and helps to restore the fever response. Components of these approaches to treatment have also been independently studied in hundreds of clinical trials conducted at research centers worldwide.
SAFETY AND EFFECTIVENESS
Hyperthermia has been studied for the treatment of chronic pain, recurrent respiratory infections, asthma, urinary tract infections, and immune deficiency. Induced hyperthermia was first evaluated in animal models 35 years ago, and then in humans over the past 30 years, both in cancer patients and in healthy volunteers.[16] [17] [18] Initial studies explored the most effective ways to administer the therapy, defining the length of treatment,[19] heat sources,[20] optimal temperatures,[21] and the effects produced. Treatment has been applied as a free-standing therapy, in combination with immune therapies such as dendritic cell injections,[22] and in tandem with conventional therapies such as radiation,[23] chemotherapy,[24] or hormone therapy.[25] Two decades of research have shown that hyperthermia is a safe procedure for the greater majority of patients and for many types of cancer.xvi-xvii
Treatment without any side effects. Researchers at the Roswell Park Cancer Institute in Buffalo, New York report that total-body hyperthermia treatments are “well-tolerated, with no significant adverse events related to cardiac, hepatic, renal, or pulmonary systems.” xviii A German study of hyperthermia for pain in fibromyalgia patients tracked safety and effectiveness. “Side effects were observed in 14 of 69 participants (20%) but all disappeared in less than 30 minutes.”[26] The study found that hyperthermia combined with standard multimodal rehabilitation was significantly more effective than standard therapy alone in terms of reducing pain intensity while improving quality of life.
Contraindications. At the Medical Center Cologne, total-body hyperthermia is provided to approximately 90% of all patients. Patients with a history of heart disease or brain tumors must be carefully screened. Because total body hyperthermia can cause a certain amount of stress to the system, it is usually not provided to patients with documented cardiac decompensation or those with brain cancer because the therapy can potentially evoke cardiac difficulties or an epileptic seizure. For almost all other patients, total-body hyperthermia has no known negative side effects.
Effectiveness. Hyperthermia is effective in activating Natural Killer cells (NK cells), which play an important role in destroying malignant cells. .[27] T-cells are also enlisted to destroy cancer using a novel approach. To engage T-cells, dendritic cells are cultured from the patient’s own white blood cells and then injected the following hyperthermia as shown in Figure 2. These dendritic cells have an antigen-presenting function—they hold in “memory” the identity (antigen profile) of the malignant cells. A small injection conveys millions of vital, activated dendritic cells, which then education the patient’s T-cells to search and destroy abnormal malignant cells. In combination, the increased number of dendritic cells, activated T-cells, and NK cells have inhibitory effects on tumor growth.[28]
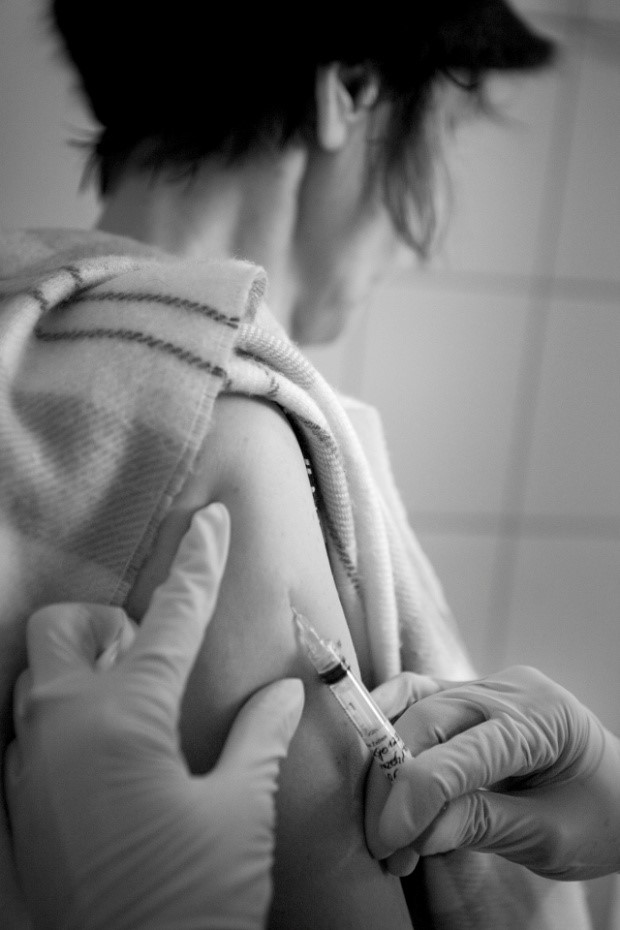
Figure 2. Patient receiving a dendritic cell injection. Reproduced by permission from, Gorter, R. and Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment. Berkeley: North Atlantic Books
Once the immune system is engaged, the body begins destroying cancer cells from within. This reduces the need for medication and stabilizes the body against further deterioration. These gains provide the basis for a sense of well-being in the patient and improve health, and healing, even in many patients with stage III and IV cancers. In a broad review of the literature, the majority of studies reported a stabilizing therapeutic response in more than 50% of patients who received whole-body hyperthermia—typically 56% to 80% of those treated.
Hyperthermia and conventional treatment. Both whole-body hyperthermia and regional hyperthermia increase the success rate of radiationxxiii and chemotherapyxxiv without affecting the activity of the medication. This combination therapy often results in fewer side effects than chemotherapy or radiation alone. A study conducted at a medical center in the Netherlands tracked the progress of 378 cancer patients receiving hyperthermia in combination with radiation treatments. Over an 8-year time period, a positive response was achieved in 77% of patients. At 5 years, the disease-specific survival rate was 47%, which is exceptional in cancer treatment. Toxicity was an issue for 12% of patients. Researchers concluded that in addition to diagnosis, “the number of hyperthermia treatments emerged as a predictor of positive outcome.” xxvi

One of the staff physicians, Dr. Montassar Cherif, checking the patients during a
“fever-range, total-body hyperthermia” session at MCC
THE GORTER HYPERTHERMIA PROTOCOL
The approach to hyperthermia at the Medical Center Cologne is based on 35 years of clinical experience, carefully calibrating every aspect of the procedure for maximum safety and benefit. The protocol has been described in detail in the book, Fighting Cancer-A Non-toxic Approach to Treatment. This model differs from other treatment protocols in several ways:
- Temperatures are more moderate (“fever-range, total-body” hyperthermia)
- State-of-the-science equipment is used
- Dendritic injections of cultured white blood cells (monocytes) are provided at specific timed intervals usually directly after hyperthermia
- An individualized program of integrative therapies is developed for each patient
Safety. Studies conducted in the 1980s and beyond have established hyperthermia as a safe form of treatment.xvi-xvii The therapy is accomplished with almost no disruption or side effects—patients typically experience less than one day of mild flu-like symptoms. Once patients complete the hyperthermia treatment, they feel cleansed and energized. In many cases, this treatment is provided as the first stage of the protocol to engage the immune system.
- Monitoring – The patient’s heart rate and oxygen saturation are monitored at all times.
- Hydration – Safety measures used in Cologne include an electrolyte IV solution throughout the procedure to avoid dehydration.
- Heat source – Infrared radiation serves as a safe, optimal heat source.[29] The electro-hyperthermia equipment was developed by the German company “Celsius 42” (Siemens).
Protocol. The patient lies within a tent-like hyperthermia chamber with their head outside the chamber. Their body is heated by specially designed infrared lamps. Infrared consists of invisible light waves close to those of visible light on the spectrum and is the primary form of energy received from the sun. The infrared rays warm blood vessels close to the surface of the skin. As the temperature in the skin rises, the temperature of blood in surface capillaries increases, circulation increases, and the warmth spreads throughout the body.
With the increase of core temperature, the patient begins to perspire. However, in the closed hyperthermia chamber, evaporation is reduced as shown in Figure 3.. Transpiration and perspiration lead to cooling only when water can be evaporated. Without the process of evaporative cooling, the body temperature continues to increase, raising core temperature, and inducing a fever-like state. Once the temperature of 103o F/39.5o C is achieved and maintained for one to two hours, the fever is gradually reduced over the course of another hour or two.
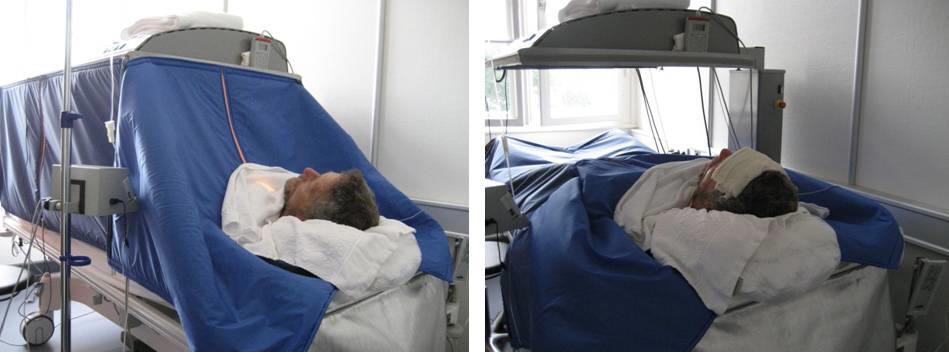
Figures 3 and 4. Erik Peper receiving hyperthermia at Medical Center Cologne, in order to document the treatment for the book, Fighting Cancer. Note in the picture on the right, the chamber has been opened to allow perspiration, and the nurse has placed a cool cloth on his forehead to make him more comfortable during the cooling down period. Reproduced by permission from, Gorter, R. and Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment. Berkeley: North Atlantic Books
Moderating temperature. Controlled fever is maintained at a moderate temperature to safeguard the well-being of the patient. Maximum temperatures range from 101 F (38.5 C) to 103 F (39.5 C). In contrast to the Gorter Model, many of the research studies use maximum temperatures in the range of 41.8 to 42 C (107.5 F). In some studies, patients were anesthetized so they could tolerate the high temperatures. Unnecessary anesthesia is always to be avoided since it can induce senility in older patients, a phenomenon known as Sundowner Syndrome. General anesthesia is also frequently immune-suppressive, and therefore should be minimized or avoided with cancer patients.)
Integrative therapies: “Translational Medicine”. At the Medical Center Cologne, total-body hyperthermia is usually provided in combination with local hyperthermia, injections of dendritic cells, mistletoe injections, IV nutrients for immune restoration, and other immune therapies.
Following total-body hyperthermia, an injection of dendritic cells cultured from the patient’s own white blood cells is injected into the skin. After the injection, patients typically experience mild flu-like symptoms for 6 to 12 hours. These symptoms indicate the activation of the body’s healing response. Once the symptoms subside, almost all patients report less pain than before the treatment and a sense of well-being. It has been observed that patients who react with flu-like symptoms after the vaccination with dendritic cells clearly do better and show more benefit from the therapy than those patients who do not mount a flu-like response. All patients who achieved complete remission experienced flu-like symptoms.
Gorter Treatment Outcomes: Breast Cancer
The following outcomes data summarizes follow-up for 292 Medical Center Cologne patients with stages IIIb and IV advanced metastatic breast cancer (patients who had been advised that they had no further standard treatment options). Typical integrative treatment for breast cancer includes local hyperthermia, whole-body hyperthermia, dendritic cell therapy, mistletoe and other types of immunotherapy, lifestyle changes including improved dieting. All patients had at least three cycles of dendritic cell therapy.
|
Advanced stage IIIb – IV metastatic breast cancer patients, 16 yrs after treatment, N=292
15% (N=45) 100% complete remission 53% (N=156) >50% (partial) remission and significantly prolonged life expectancy or still alive 17% (N=50) progression of cancer and death 14% (N=41) lost to follow-up
|
Case History: Breast Cancer
“When I was diagnosed with malignancies for the fourth time, I decided to go to Germany for treatment at the Cologne Medical Center. I had been diagnosed with breast cancer in 1999 and one of my breasts was surgically removed at that time, but I declined radiation or chemotherapy. After careful thought, I decided to do non-toxic follow-up treatment, but I also went back to the hospital for periodic check-ups. For the next six years, I was in remission. But at that point, I developed bone cancer. I beat it a second time, but cancer came back again.
That is when I went to see Dr. Gorter. I improved very quickly with the treatment at Cologne—a combination of hyperthermia, immune restoration, and dendritic cell therapy. The pain disappeared very quickly and I was soon pain-free. Walking had become difficult and I even walked with a cane for a while, because moving hurt so much. With this treatment, the pain remains gone and I can walk again. Not all the tumors are gone. Bu the pain is gone and I feel good about it”
Ledge Abbenhuis, Belgium, a nine-year survivor of breast cancer with a history of recurring bone, brain, and liver metastasis
LOCALIZED (REGIONAL) HYPERTHERMIA
Localized heat treatment is another approach used in the Gorter Model with all patients who have solid tumors. In this therapy, heat is initiated only in the tumor cell, leaving healthy cells unaffected (see Figure 4).
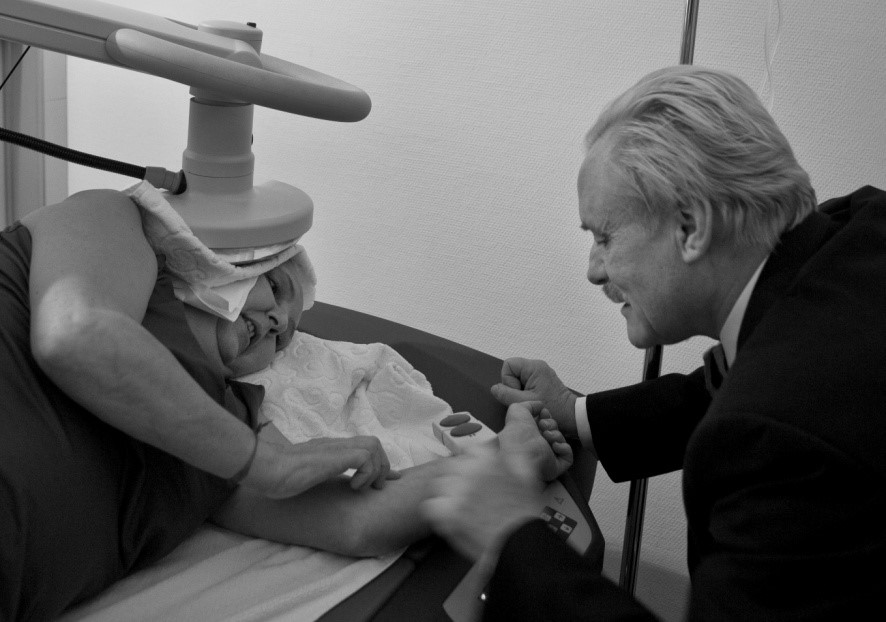
Figure 4. The patient is being treated by Dr. Gorter with local hyperthermia for brain cancer (photo by Jan Asenbrennerova). Reproduced by permission from, Gorter, R. and Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment. Berkeley: North Atlantic Books
Safety protocol. The electro-hyperthermia equipment used for localized hyperthermia causes no risk of burns and can be focused exclusively on any area of the body. Tumor cells are heated selectively as tumor cells have a much higher electromagnetic resistance than regular cells. This enables us to provide interventions for areas of the body that would normally be difficult to treat such as the head, lungs, and bone tissue. The fact that hyperthermia can be efficacious in treating brain tumors was borne out by a recent phase III study for patients with brain lesions, in which hyperthermia proved to support significantly better results in illness-free time and survival when compared with radiation and/or medication alone.
Mechanism. Tumor cells produce abnormal tumor-specific proteins which are thousands of times larger than normal proteins. During hyperthermia, these tumor proteins absorb energy when exposed to an MRI-like electromagnetic field. This causes the malignant cells to heat up to an extremely high-temperature of 107.6°F (42°C). The heating causes the cancer cells to increase their metabolism and lactic acid production. As metabolism speeds up within the tumor cells, they essentially self-destruct and drown in the lactic acid they produce, resulting in cell death (necrosis). Neighboring healthy cells are unaffected and remain at normal body temperature. Localized hyperthermia is provided to approximately 99% of patients at the Medical Center Cologne and is currently also available in the United States at Cancer Treatment Centers of America.
Research. To date, there are more than 3500 articles in the medical literature listed under “regional hyperthermia.” In conventional oncology, the majority of studies have evaluated local hyperthermia in combination with chemotherapy or radiation. Over 330 clinical trials have been conducted in countries worldwide, across Europe, and in Asia and Israel. Extensive research has been performed at the National Cancer Research Center in Heidelberg in Germany for more than two decades and at the National Cancer Institute in Rome. American studies include research at the Anderson Cancer Center in Houston, at Duke, and at Wake Forest.
Integrative treatment. Localized hyperthermia is a highly effective means of destroying cancer cells without causing toxicity, particularly when used in conjunction with other immune-supportive therapies such as vitamin C infusions, thymus peptides, and mistletoe extract. In addition, most patients are provided with dendritic cell injections since the heating process makes cancer cells more vulnerable to destruction by the immune system. One could also say that the Gorter Model is a perfect example of Translational Therapy (from bench to bed)

Teun van Vliet survives 20 years of recurrent GBM
Gorter Treatment Outcomes: Brain Cancer
At the Medical Center Cologne, even patients with primary or secondary brain tumors or metastases of the breast or lung are successfully treated without any side effects using this approach. The research shows that 46% of all patients with stage IV Glioblastoma multiforme go into complete, long-term remission, following a protocol of at least 3 dendritic cell vaccinations and 24 sessions of local hyperthermia. This is a very promising outcome since with conventional treatment approximately 72% of patients with brain tumors (Glioblastoma multiforme stage IV) die within the first year after diagnosis and only 1-3% survive up to three years.
Localized hyperthermia clinical trials. Almost 300 clinical trials have been published to date on “regional” or “localized” hyperthermia. Among 50 recent clinical trials, 60% of the studies involved the use of hyperthermia with chemotherapy. The majority of the other studies evaluated localized hyperthermia with surgery or radiation. A third group evaluated hyperthermia with immunotherapy (primarily TNF-). Combining any of these therapies with localized hyperthermia appears to be more effective with few side effects. Only a handful of large clinical trials have focused on localized hyperthermia as a stand-alone treatment, perhaps due to the lack of economic incentives.

Teun van Vliet World Champion cycling and Tour de France.
Case History: Brain Cancer (recurrent Glioblastoma multiforme stage IV)
Twenty years ago, Teun van Vliet was twice an indoor world champion cyclist and in 1988 wore the yellow jersey in the Tour de France. In 2001, he was diagnosed with a brain tumor and in 2006 an inoperable recurrence of the tumor was detected. Teun had another round of brain surgery (“debulking”) and also received chemotherapy in combination with radiation treatment. This caused him to lose his power of speech, and to some degree, he also lost memory and coordination. Within conventional oncology, nothing more could be done for him and he was told that he had less than half a year left to live. Teun and his partner decided to seek a second opinion and they went to Cologne to consult with Dr. Gorter, who advised him to try localized hyperthermia in combination with immune therapy. Teun’s partner soon reported beneficial changes in his health:
“The first thing we noticed about these treatments was that they really improved his speech. He is much more lively; more active and makes jokes again. I have my old buddy back, really. When he comes home from Cologne, his speech has improved, his motor skills have improved, he feels more energetic. Nothing but improvements. The quality of his life is definitely better.”
Teun van Vliet, Tour de France champion cyclist, a patient at the Medical Center Cologne, and survivor of stage IV brain cancer. In April 2012, a new MRI scan confirmed that there is still no recurrence of cancer and Teun has been clinically cancer-free for more than 6 years. In 2020, Teun is still kicking and doing well….
The Importance of an Integrative Approach
We believe (and our data show) that the noninvasive support provided by the Gorter Model protocol is not only an ideal adjunct to many treatment programs, because it does not increase the level of toxicity in the body or the immune burden; nor is it invasive. Hyperthermia can be provided in combination with a range of other therapies, both integrative and conventional but also can still help hospice patients to go into complete remission and live decades longer. Approx. 94% of all patients who came for treatment according to the “Gorter Model” where patients with less than 3 months life expectancy and (in the beginning) often had to come for treatment in an ambulance. Thus; as they had received all treatments options available, they participated in the treatment of the Gorter Model protocol only.
What makes this approach unique is the calibrated timing of hyperthermia and the dendritic cell vaccinations, which are augmented with other elements of the program, such as IV antioxidants and subcutaneous mistletoe injections. The favorable outcomes indicate that in this protocol, the sum of the whole is greater than the parts. This form of treatment does not promise a cure, but it does offer the possibility of improvement. The majority of stage IV patients experience significantly longer survival with a greater quality of life; quite a few go in complete remission up to 18 years now.
Several other elements contribute to the success of this therapy. The program tends to attract patients who are proactive: they chose to seek help, and they have a will to live. In addition, Dr. Gorter serves as a good role model, because he is a cancer survivor. This provides the non-verbal cue that hope is possible. Much of what he is suggesting to patients, he has actually experienced and applied in his own healing.
We predict that the next phase of this integrative (translational) approach will focus on patients at a much earlier stage in disease progression. Given the low toxicity and the potential effectiveness of immunotherapy, this treatment would be highly appropriate for patients who are advised to observe watchful waiting.

Robert Gorter, MD, PhD. (l) and Erik Peper PhD. (r) scrutinizing their own texts for the next edition
*About Robert Gorter, MD, PhD
Dr. Gorter trained in Amsterdam and for 10 years served the Dutch community as a physician, lecturer, and researcher. Then, on request of a patient-based foundation “Michael Group” he immigrated to the USA and became involved in the HIV/AIDS care at “Ward 86” at San Francisco General Hospital of the University of California San Francisco (UCSF), a Department which provided world leadership in defining and treating AIDS. Dr. Gorter became the medical director of the Department of AIDS Epidemiology and Biostatistics, University of California, San Francisco Medical School. He has spent the past 50 years applying lessons learned from the AIDS epidemic and his own survival of end-stage Germ Cell Carcinoma without any operation, radiation, or chemotherapy (1975) and the emerging field of immunotherapy in the treatment of cancer. Dr. Gorter served as a full UCSF faculty member from 1984 until 2012. Parallel, as a senior lecturer, he taught at San Francisco State University from 1984 to 2020. He also holds a PhD from the University of Witten/Herdecke in Germany in 1993, where he continues to serve as a full faculty member. He holds a medical degree in conventional Western medicine with post-doctoral work in the U.S. He has also completed specialty training in Anthroposophical medicine in Switzerland with an emphasis on oncology. For additional biographical information on Dr. Gorter, see the section on Development of the Gorter Model, earlier in this article. For more information on the Gorter Model, see:
www.gorter-model.org and www.youtube.com/user/mccfilip
**About Erik Peper, PhD
Erik Peper is an internationally known expert on holistic health, stress management, and biofeedback. He received his BA from Harvard University in 1968 and his Ph.D. in psychology from Union Graduate Institute in 1975. Since 1976 he has taught at San Francisco State
University (SFSU), where he has been instrumental in establishing the Institute for Holistic Health Studies, the first program in holistic health at a public university in the U.S. Dr. Peper is president of the Biofeedback Foundation of Europe, and former president of the Biofeedback Society of America (Association for Applied Psychophysiology and Biofeedback). A sports psychologist for the U.S. Olympic Gymnastic Team for four years, his expertise includes peak performance and stress management. He is also a recognized expert on workplace health, and computer-related injuries and received a State of California Governor’s Employee Safety Award in 2004 for his work within these areas.
Dr. Peper has written published than 200 articles and nine books, including Make Health Happen, Biofeedback Mastery: An Experiential Teaching and Self-Training Manual, and Fighting Cancer: A Nontoxic Approach, coauthored with Dr. Gorter. In addition to teaching, research, consulting, and travel, he maintains a biofeedback practice in Berkeley, California. For information see: www.biofeedbackhealth.org and his blog site, www.peperperspective.com
References
[1] Adapted from: Gorter, R. and Peper, E. (2011). Fighting Cancer-A Nontoxic Approach to Treatment, Berkeley: North Atlantic Books ISBN 978-1-58394-248-2.
[2] Oehler R, et al. Cell type-specific variations in the induction of hsp70 in human leukocytes by feverlike whole-body hyperthermia. Cell Stress Chaperones. 2001 Oct;6(4):306-315.
[3] Kleef R, Jonas WB, Knoller W, Stenzinger W. Fever, cancer incidence, and spontaneous remissions. Neuroimmunomodulation. 2001;9(2):55-64.
[4] Kleef, R. & Hager, D. Incidence of Malignancies and Missing History of Fever in Baronzio, G.F. & Hager, E. (2006). Hyperthermia in Cancer Treatment: A Primer. New York: Springer US.
[5] Laurence JZ. The diagnosis of surgical cancer (Lister Prize say for 1854). London: Churchill. 1854; 56.
[6] Ralf Kleef and E. Dieter Hager. Fever, Pyrogens, and Cancer. NCBI. Bookshelf » Madame Curie Bioscience Database, Oncology. Published 20__. Available at http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=eurekah&part=A59581. Accessed 07-14-10.
[7] Remy W, Hammerschmidt K, Zänker KS. et al. Tumorträger haben selten Infekte in der Anamnese [in ….]. Med Klinik. 1983; 78: 95–98.
[8] Kölmel K, Gefeller O, Haverkamp B. Febrile infections and malignant melanoma: Results of a case-control study. Melanoma Res. 1992; 2: 207–211.
[9] Schlehofer B, Blettner M, Becker N. et al. Medical risk factors and development of brain tumors. Cancer. 1992; 69: 2541–2547.
[10] Schulman, C.I., Namias, N., Doherty, J., Manning, R.J., Li, P., Elhadded, A., Lasko, D., Amortegui, J., Dy, C.J., Diugash, L, Baracco, G., & Cohn, S.M. (2005). The effect of antipyretic therapy upon outcomes in critically ill patients: a randomized, prospective study. Surg. Infect., 6(4), 369-375.
[11] Barlow G., Lillie, P., Nathwani, D. & Davey. (2010). Fever as nature’s engine-Some some clinical data. BMJ;340: doi:10.1136/BMJ.c905
[12] Ader, R., & Cohen, N. (1975). Behaviorally conditioned immunosuppression. Psychosomatic medicine.37(4), 333-340.
[13] Ader, R. (2003). Conditioned immunomodulation: research needs and directions. Brain Behav Immun. 17, Suppl 1, S51-7.
[14] Goebel, M.U., Trebst, A.E., Steiner, J., Xie, Y.F., Exton, M.S., Frede, S., Canbay, A., Michel, M.C., Heeman, U., & Schedlowski, M. (2002). Behavioral conditioning of immunosuppression is possible in humans. The FASEB Journal,16, 1869-1873.
[15] Hiramoto, R., Rogers, C., Demissie, S., Hsueh, C, M., Hiramoto, N., Lorden, J. & Ghanta, V. (1996). The use of conditioning to probe for CNS pathways that regulate fever and NK cell activity. Int J Neurosci. 84(1-4):229-45.
[16] Dietzel F. Basic principles in hyperthermic tumor therapy. Recent Respite Cancer Res. 1983;86:177-190.
[17] Kerner T, et al. Whole-body hyperthermia: a secure procedure for patients with various malignancies? Intensive Care Med. 1999 September;25(9):959-965.
[18] Kraybill WG, et al. A phase I study of fever-range whole-body hyperthermia (FR-WBH) in patients with advanced solid tumors: correlation with mouse models. Int J Hyperthermia. 2002 May-Jun; 18(3):253-266.
[19] Atanackovic D, et al. Patients with solid tumors treated with high-temperature whole-body hyperthermia show a redistribution of naïve/memory T-cell subtypes. Am J Physiol Regul Integr Comp Physiol. 2006 Mar;290(3): R585-594. Epub 2005 Oct 27.
[20] Wehner H, von Arden A, Kaltofen S. Whole-body hyperthermia with water-filtered infrared radiation: technical-physical aspects and clinical experiences. Int J Hyperthermia. 2001 Jan-Feb; 17(1):19-30.
[21] Doering TJ, et al. Cerebral autoregulation during whole-body hyperthermia and hyperthermia stimulus. Am J Phys Med Rehabil. 1999 Jan-Feb; 78(1):33-38.
[22] Bedrosian I, et al. Intranodal administration of peptide-pulsed mature dendritic cell vaccines results in superior CD8+ T-cell function in melanoma patients. J Clin Oncol. 2003 Oct 15;21(20):3826-3835.
[23] Francona M, et al. Radiotherapy and hyperthermia for treatment of primary locally advanced cervix cancer: results in 378 patients. Int J Radiat Oncol Biol Phys. 2009 Jan 1;73(1):242-25-. Epub 2008 Nov 5.
[24] Bull, JM, et al. Fever-range whole-body thermal therapy combined with cisplatin, gemcitabine, and daily interferon-alpha: description of a phase I-II protocol. Int J Hyperthermia. 2008 Dec;24(8):649-662.
[25] Kappel M, et al. Somatostatin attenuates the hyperthermia-induced increase in neutrophil concentration. Euro J Appl Physiol Occup Physiol. 1998;77(1-2):149-56.
[26] Brockow T, Wagner A, Franke A, Offenbacher M, Resch KL. A randomized controlled trial on the effectiveness of mild water-filtered near-infrared whole-body hyperthermia as an adjunct to a standard multimodal rehabilitation in the treatment of fibromyalgia. Clin J Pain. 2007 Jan; 23(1):67-75.
[27] Kappel M, Poulsen TD, Galbo H, Pedersen BK. Influence of minor increases in plasma catecholamines on natural killer cell activity. Horm Res. 1998:49(1):22-26.
[28] West P, et al. Feasibility and analysis of thermal parameters for the whole-body-hyperthermia system IRATHERM-2000. Int J Hyperthermia. 2000 Jul-Aug;16(4):325-339.
[29] Zellner M, et al. Human monocyte stimulation by experimental whole-body hyperthermia. Wien Klin Wochenschr. 2002 Feb 15;114(3):102-107.




