Remarkable similarities for the 2020 and 2018 flu season:
Contrary to the assertions of Dutch politicians, the differences do not show any grounds for taking draconian measures, which are admittedly causing much more damage.
by
Maurice de Hondt, PhD, and Robert Gorter, MD, PhD.
October 05, 2020
In this article, I compare the death rate in the 2019-2020 flu season with that of 2017-2018. The absolute number in 2020 has increased slightly compared to 2018, but this can be attributed to the fact that the population has grown somewhat older on average in those two years.
Every week, the Rijksinstituut voor Volksgezondheid en Milleu (RIVM) in the Netherlands publishes an overview of the mortality figures per week and per flu season. They show clearly how the COVID-19 period relates to previous four flu seasons. In order to also take into account under-mortality, the period from week 40 runs from one year to week 39 of the following year.
In the last four seasons, the death rate was between 150,000 and 160,000. We compared the 2019-2020 season (hereinafter: 2020) with 2017-2018 (hereinafter: 2018). In 2018, in the Netherlands, but also Europe at large, had a severe flu wave.
In 2020, 160,500 people died. The death rate in 2018 was 153,400. The increase of 7,100 deaths can only be assessed if the change in the population composition in those two years is first considered.
By comparing three age groups, one gets a clearer picture of the differences.
– Under the age of 65 the mortality rate is roughly the same: approximately 21,000 of the 14 million people died.
– About 2.5 million inhabitants are between 65 and 79 years old. In that age group, between 45,000 and 50,000 people died. In 2020 this was 3,200 more than in 2018.
– Above 80 years there are about 800,000 people. More than 90,000 of these died. Compared to 2018, this is 4,300 more.
At first glance, it appears that there has been an increase of 7,500 deaths. But if one zooms in on the three different age groups, a completely different picture emerges.
The age category of people over 80 has grown in two years by no less than 45,000 people (an increase of more than six percent). And if that growth is included in the calculation, there is even a small decrease compared to 2018 in relative terms.
– In the 65-79 group, the number of inhabitants increased by about five percent. If you include that growth in the calculation, the increase in the number of deaths is approximately 1,000.
– The group under 65 has grown the least at half a percent. The relative mortality in that group compared to 2018 has even decreased slightly.
If one adds up the relative mortality in the three age groups, one arrives at approximately zero.
The graphs below show the mortality rate per week for three age groups. The data starts in week 40, but the chart starts in week two. Note: Each graph has a different scale (the cumulative death rate). The similarities between those two years can easily be deduced from this.
We leave aside what these figures would have looked like if there had not been a lockdown in mid-March 2020.

In conclusion, the development of excess mortality in the Netherlands can be compared with Sweden, as can be seen on the site of the FT. The red numbers indicate the difference compared to the previous four years because the measures in Sweden were less stringent than in the Netherlands. These mortality rates have not been corrected for the shift in age groups. The small equity in the Netherlands is related to the heat wave in August.
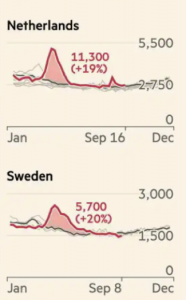
The increase in Sweden was less high and the decline more gradual. Sweden is currently in a phase of under-mortality.
When comparing with Sweden, it is important to bear in mind that the age distribution in the Netherlands is very similar to that of Sweden and that population growth there is slightly faster than in the Netherlands.
Once can wonder why there is a global trend among politicians and experts liked to them to declare Second and Third and fourth waves to come or…. global mandatory vaccinations against COVID-19 and all future flue epidemics (remember the Mexican flu and other killer epidemics?)
Below just one very recent article by the NEJM on mandatory vaccinations as only solution.
Ensuring Uptake of Vaccines against SARS-CoV-2
Mello et al. wrote the following in the New England Medical Journal of Medicine (NEJM) published online on October 1st, 2020. (This article was published earlier on June 26, 2020, at NEJM.org. but appeared online on October 1st, 2020.
COVID-19 (SARS-CoV-2) continues to present a heavy toll and the development of a vaccine appears the most promising means of restoring normalcy to civil life. Perhaps no scientific breakthrough is more eagerly anticipated. But bringing a vaccine to the market is only half the challenge; also critical is ensuring a high enough vaccination rate to achieve herd immunity. Concerningly, a recent poll found that only 49% of Americans planned to get vaccinated against SARS-CoV-2.(1)
One option for increasing vaccine uptake is to require it. Mandatory vaccination has proven effective in ensuring high childhood immunization rates in many high-income countries. However, except for influenza vaccination of health care workers, mandates have not yet been widely used for adults.
Although a vaccine remains months to years away, developing a policy strategy to ensure uptake takes time. Already today the authorities must develop a strategy to help ensuring uptake by the general population of the vaccine when it becomes available — including consideration of when a mandate might become appropriate. Our approach is guided by lessons from U.S. experiences with vaccines for the 1976 “swine flu,” H1N1 influenza, smallpox, and human papillomavirus (HPV).
Mello et al. propose that six substantive criteria should be met before country imposes a SARS-CoV-2 vaccine mandate (see box).
The first is the existence of evidence that Covid-19 is inadequately controlled by national authorities by other measures, such as testing, contact tracing, and isolation and quarantine — as indicated by sustained, troubling trends in new cases, hospitalizations, or deaths. Principles of public health law and ethics require that interventions that impinge on autonomy be reasonable and necessary; therefore, COVID-19 must present an ongoing threat. By the time a vaccine is available more will be known about natural immunity in the population, the consequences of relaxing community mitigation measures, and the feasibility of scaling up test-and-trace strategies. There should be a reasonable indication as to whether further and stricter measures are needed.
Six Criteria for Mandatory Vaccinations on a National (Global?) Scale for COVID-19 and Other Future Epidemics
1) Covid-19 is not adequately contained in a country or globally;
2) National health authorities must determine which risk groups must be vaccinated or the country at large;
3) The supply of vaccine(s) must be sufficient to cover the risk groups or the general population at large to guarantee a general mandatory vaccination;
4) Available evidence about the safety and efficacy of the vaccine has been transparently communicated.
5) The country has created an infrastructure to provide access to vaccination without financial or logistic barriers, compensation to workers who have adverse effects from a required vaccine, and real-time surveillance of vaccine side effects.
6) In a time-limited evaluation, voluntary uptake of the vaccine among high-priority groups has fallen short of the level required to prevent epidemic spread.
The authors argue that when voluntary vaccinations against COVID-19 or other infectious entities fall short, mandatory global vaccinations must be put in place to protect the population against itself.
Dr. Robert Gorter: it is striking that, although the authors wrote very carefully and weighed their words well to explain when and why a general (global?) mandatory vaccination program would be needed, their article prepares the reader to be prepared to accept mandatory vaccinations in the (near) future.
Authors: Michelle M. Mello, J.D., Ph.D., Ross D. Silverman, J.D., M.P.H., and Saad B. Omer, M.B., B.S., M.P.H., Ph.D.
This article was published on June 26, 2020, at NEJM.org. but appeared online on October 1st, 2020.
Author Affiliations
From Stanford Law School and Stanford Health Policy and the Department of Medicine, Stanford University School of Medicine, Stanford, CA (M.M.M.); the Department of Health Policy and Management, Indiana University Richard M. Fairbanks School of Public Health, and the Indiana University Robert H. McKinney School of Law, Indianapolis (R.D.S.); and the Yale Institute for Global Health and the Yale Schools of Medicine, Public Health, and Nursing, New Haven, CT (S.B.O.).
References
- Associated Press-NORC Center for Public Affairs Research. Expectations for a COVID-19 vaccine. May 2020 (http://www.apnorc.org/projects/Pages/Expectations-for-a-COVID-19-Vaccine.aspx. opens in new tab). Google Scholar
- Trogen B, Oshinsky D, Caplan A. Adverse consequences of rushing a SARS-CoV-2 vaccine: implications for public trust. JAMA 2020;323:2460-2461.
- Hartocollis A, Chan S. Flu vaccine requirement for health workers is lifted. New York Times. October 23, 2009.
- DeRoo SS, Pudalov NJ, Fu LY. Planning for a COVID-19 vaccination program. JAMA 2020;323:2458-2459.
- Mello MM, Abiola S, Colgrove J. Pharmaceutical companies’ role in state vaccination policymaking: the case of human papillomavirus vaccination. Am J Public Health 2012;102:893-898.