by
Robert Gorter, MD, PhD, is emeritus professor of the University of California San Francisco Medical School (UCSF)
Introduction to CBD and Osteoporosis
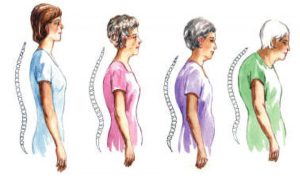
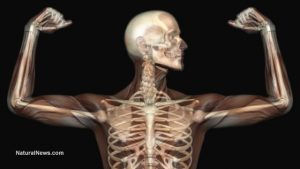
Osteoporosis is a bone diseases characterized by a loss of bone mass, leading to skeletal fragility and fractures. One of two women and one of eight men will be diagnosed with osteoporosis. It is called a “silent disease” because you cannot feel or see your bones becoming thinner over time. Unfortunately, many people are diagnosed with osteoporosis only after a painful fracture has occurred. All older adults are at risk but certain individuals have factors that can increase their chance of developing the disease.
Osteoporosis is a usually preventable decalcification of bone and always leads to significant symptoms and diseases, decreased life expectancy and decreased quality of life.
Dr. Gorter offers his knowledge and view on osteoporosis and how it can be prevented in most cases with CBD. In addition, Dr. Gorter explains the modes of action of CBD and makes understandable all the positive effects in aging.
Osteoporosis decreases the life expectancy in women by approx. six years and in men by approx. four years; and it affects all elderly people in their quality of life and independence. With a greying population, where the elderly life longer, osteoporosis is becoming a major economic factor and costs society hundreds of billions of US Dollars or Euros per year.
In this article, as a Cannabis sativa L. expert since 1971, Dr. Gorter discusses the efficacy of CBD in treatment and prevention of osteoporosis. CBD has no side effects and is very low in costs.

Elderly woman with osteoporosis showing the characteristic curved back from compression fractures of her back bones.
March 25th, 2018
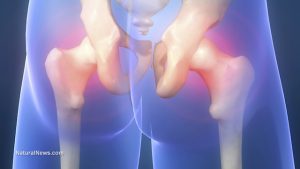
Osteoporosis is a disease where increased bone weakness increases the risk of a broken bone. It is the most common reason for a broken bone among the elderly. Bones that commonly break include the vertebrae in the spine, the bones of the forearm, and the hip. Until a broken bone occurs there are typically no symptoms. Bones may weaken to such a degree that a break may occur with minor stress or spontaneously. Chronic pain and a decreased ability to carry out normal activities usually occur following a broken bone.
Osteoporosis may be due to lower than normal bone mass and greater than normal bone loss. Bone loss increases after menopause due to lower levels of estrogen. Osteoporosis may also occur due to a number of diseases or treatments including alcoholism, anorexia, hyperthyroidism, kidney disease, and surgical removal of the ovaries. Several prescribed medications increase the rate of bone loss including some anti-seizure medications, chemotherapy, proton pump inhibitors, selective serotonin reuptake inhibitors, Non-Steroidal Anti-Inflammatory drugs and steroids. Not enough exercise and smoking are also risk factors. Osteoporosis is defined as a bone density of 2.5 standard deviations below that of a young adult. This is typically measured by dual-energy X-ray absorptiometry at the hip or hand.
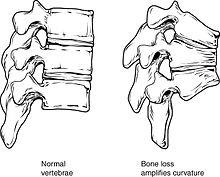
Osteoporosis is an age-related disorder that causes the gradual loss of bone density and strength. When the thoracic vertebrae are affected, there can be a gradual collapse of the vertebrae. This results is kyphosis, an excessive curvature of the thoracic region
Prevention of osteoporosis includes a proper diet during childhood and efforts to avoid the numerous medications that cause the condition. Efforts to prevent broken bones in those with osteoporosis include a good diet, exercise, and fall prevention and Cannabidiol (CBD). Lifestyle changes such as stopping smoking and not drinking alcohol always help. Biphosphonate-containing medications are useful in those with previous broken bones due to osteoporosis or in bone metastases.
Osteoporosis becomes more common with age. About 15% of white people in their 50s and 70% of those over 80 are affected. It is more common in women than men. In the developed world, depending on the method of diagnosis, 2% to 8% of males and 9% to 38% of females are affected. Rates of disease in the developing world are unclear. About 22 million women and 5.5 million men in the European Union had osteoporosis in 2010. In the United States in 2010 about eight million women and one to two million men had osteoporosis. Caucasians and Asian people are at greater risk. The word osteoporosis is from the Greek terms for “porous bones”.
Osteoporosis itself has no symptoms; its main consequence is the increased risk of bone fractures. Osteoporotic fractures occur in situations where healthy people would not normally break a bone; they are therefore regarded as fragility fractures. Typical fragility fractures occur in the vertebral column, rib, hip and wrist.
Fractures
Fractures are the most dangerous aspect of osteoporosis. Debilitating acute and chronic pain in the elderly is often attributed to fractures from osteoporosis and can lead to further disability and earlier mortality. These fractures may also be asymptomatic. The most common osteoporotic fractures are of the wrist, spine, shoulder and hip. The symptoms of a vertebral collapse (“compression fracture”) are sudden back pain, often with radicular pain (shooting pain due to nerve root compression) and rarely with spinal cord compression or cauda equina syndrome. Multiple vertebral fractures lead to a stooped posture, loss of height, and chronic pain with resultant reduction in mobility.
Risk factors
Risk factors for osteoporotic fracture can be split between non-modifiable and (potentially) modifiable. In addition, osteoporosis is a recognized complication of specific diseases and disorders. Medication use is theoretically modifiable, although in many cases, the use of medication that increases osteoporosis risk may be unavoidable. Nicotine but not caffeine is a risk factor for osteoporosis.
Non-modifiable
Bone density peaks at about 30 years of age. Women lose bone mass more rapidly than men.
The most important risk factors for osteoporosis are advanced age (in both men and women) and female sex; estrogen deficiency following menopause or surgical removal of the ovaries is correlated with a rapid reduction in bone mineral density, while in men, a decrease in testosterone levels has a comparable (but less pronounced) effect.
Race: While osteoporosis occurs in people from all ethnic groups, European or Asian ancestry predisposes for osteoporosis.
Heredity: Those with a family history of fracture or osteoporosis are at an increased risk; the heritability of the fracture, as well as low bone mineral density, is relatively high, ranging from 25 to 80%. At least 30 genes are associated with the development of osteoporosis.[26]
Those who have already had a fracture are at least twice as likely to have another fracture compared to someone of the same age and sex. Early menopause/hysterectomy is another predisposing factor.
Physique: A small stature is also a non-modifiable risk factor associated with the development of osteoporosis.
Potentially modifiable
Consumption of alcohol: Although small amounts of alcohol are probably beneficial (bone density increases with increasing alcohol intake), chronic heavy drinking increases fracture risk despite any beneficial effects on bone density.
Vitamin D deficiency: Low circulating Vitamin D is common among the elderly worldwide. Mild vitamin D insufficiency is associated with increased parathyroid hormone (PTH) production. PTH increases bone resorption, leading to bone loss. A positive association exists between serum 1,25-dihydroxycholecalciferol levels and bone mineral density, while PTH is negatively associated with bone mineral density.
Tobacco smoking (nicotine): Many studies have associated smoking with decreased bone health, but the mechanisms are unclear. Tobacco smoking has been proposed to inhibit the activity of osteoblasts, and is an independent risk factor for osteoporosis. Smoking also results in increased breakdown of exogenous estrogen, lower body weight and earlier menopause, all of which contribute to lower bone mineral density.
Malnutrition: Nutrition has an important and complex role in maintenance of good bone. Identified risk factors include low dietary calcium and/or phosphorus, magnesium, zinc, boron, iron, fluoride, copper, vitamins A, K, E and C (and D where skin exposure to sunlight provides an inadequate supply). Excess sodium is a risk factor. High blood acidity may be diet-related, and is a known antagonist of bone. Some have identified low protein intake as associated with lower peak bone mass during adolescence and lower bone mineral density in elderly populations.[4] Conversely, some have identified low protein intake as a positive factor, protein is among the causes of dietary acidity. Imbalance of omega-6 to omega-3 polyunsaturated fats is yet another identified risk factor.
High dietary protein from animal sources: Research has found an association between diets high in animal protein and increased urinary calcium, and have been linked to an increase in fractures. However, the relevance of this observation to bone density is unclear, since higher protein diets tend to increase absorption of calcium from the diet and are associated with higher bone density. Indeed, it has recently been argued that low protein diets cause poor bone health. No interventional trials have been performed on dietary protein in the prevention and treatment of osteoporosis.
Underweight/inactive: Bone remodeling occurs in response to physical stress, so physical inactivity can lead to significant bone loss. Weight bearing exercise can increase peak bone mass achieved in adolescence and a highly significant correlation between bone strength and muscle strength has been determined. The incidence of osteoporosis is lower in overweight people.
Endurance training: In female endurance athletes, large volumes of training can lead to decreased bone density and an increased risk of osteoporosis. This effect might be caused by intense training suppressing menstruation, producing amenorrhea, and it is part of the female athlete triad. However, for male athletes, the situation is less clear, and although some studies have reported low bone density in elite male endurance athletes, others have instead seen increased leg bone density.
Heavy metals: A strong association between cadmium and lead with bone disease has been established. Low-level exposure to cadmium is associated with an increased loss of bone mineral density readily in both genders, leading to pain and increased risk of fractures, especially in the elderly and in females. Higher cadmium exposure results in osteomalacia (softening of the bone).
Soft drinks: Some studies indicate soft drinks (many of which contain phosphoric acid) increase the risk of osteoporosis, at least in women. Others suggest soft drinks may displace calcium-containing drinks from the diet rather than directly causing osteoporosis.
Proton pump inhibitors (such as lansoprazole, esomeprazole, or omeprazole) that decrease stomach acid, are a risk for bone fractures if taken for two or more years, due to decreased absorption of calcium in the stomach.[53]
Medical disorders
The body regulates calcium homeostasis with two pathways; one is signaled to turn on when blood calcium levels drop below normal and one is the pathway that is signaled to turn on when blood calcium levels are elevated.
Many diseases and disorders have been associated with osteoporosis. For some, the underlying mechanism influencing the bone metabolism is straightforward, whereas for others the causes are multiple or unknown.
In general, immobilization causes bone loss (following the ‘use it or lose it’ rule). For example, localized osteoporosis can occur after prolonged immobilization of a fractured limb in a cast. This is also more common in active people with a high bone turn-over (for example, athletes). Other examples include bone loss during space flight or in people who are bedridden or use wheelchairs for various reasons.
Hypogonadal states can cause secondary osteoporosis. These include Turner syndrome, Klinefelter syndrome, Kallmann syndrome, anorexia nervosa, andropause, hypothalamic amenorrhea or hyperprolactinemia. In females, the effect of hypogonadism is mediated by estrogen deficiency. It can appear as
early menopause (<45 years) or from prolonged premenopausal amenorrhea (>1 year). Bilateral oophorectomy (surgical removal of the ovaries) and premature ovarian failure cause deficient estrogen production. In males, testosterone deficiency is the cause (for example, andropause or after surgical or chemical removal of the testes).
Endocrine disorders that can induce bone loss include Cushing’s syndrome, hyperparathyroidism, hyperthyroidism, hypothyroidism, diabetes mellitus type 1 and 2, acromegaly, and adrenal insufficiency.
Malnutrition, parenteral nutrition and malabsorption can lead to osteoporosis. Nutritional and gastrointestinal disorders that can predispose to osteoporosis include undiagnosed and untreated coeliac disease (both symptomatic and asymptomatic people), Crohn’s disease, ulcerative colitis, cystic fibrosis, surgery (after gastrectomy, intestinal bypass surgery or bowel resection) and severe liver disease (especially primary biliary cirrhosis). People with lactose intolerance or milk allergy may develop osteoporosis due to restrictions of calcium-containing foods. Individuals with bulimia can also develop osteoporosis. Those with an otherwise adequate calcium intake can develop osteoporosis due to the inability to absorb calcium and/or vitamin D. Other micronutrients such as vitamin K or vitamin B12 deficiency may also contribute.
People with rheumatologic disorders such as rheumatoid arthritis, ankylosing spondylitis, systemic lupus erythematosus and polyarticular juvenile idiopathic arthritis are at increased risk of osteoporosis, either as part of their disease or because of other risk factors (notably corticosteroid therapy). Systemic diseases such as amyloidosis and sarcoidosis can also lead to osteoporosis.
Renal insufficiency can lead to renal osteodystrophy.
Hematologic disorders linked to osteoporosis are multiple myeloma and other monoclonal gammopathies, lymphoma, leukemia, mastocytosis, hemophilia, sickle-cell disease and thalassemia.
Several inherited disorders have been linked to osteoporosis. These include osteogenesis imperfecta, Marfan syndrome, hemochromatosis, hypophosphatasia (for which it is often misdiagnosed), glycogen storage diseases, homocystinuria, Ehlers–Danlos syndrome, porphyria, Menkes’ syndrome, epidermolysis bullosa and Gaucher’s disease.
People with scoliosis of unknown cause also have a higher risk of osteoporosis. Bone loss can be a feature of complex regional pain syndrome. It is also more frequent in people with Parkinson’s disease and chronic obstructive pulmonary disease.
People with Parkinson’s disease have a higher risk of broken bones. This is related to poor balance and poor bone density. In Parkinson’s disease there may be a link between the loss of dopaminergic neurons and altered calcium metabolism (and iron metabolism) causing a stiffening of the skeleton and kyphosis.
Medication
Fractures of the long bones acutely impair mobility and may require surgery. Hip fracture, in particular, usually requires prompt surgery, as serious risks are associated with it, such as deep vein thrombosis and pulmonary embolism, and increased mortality.
Fracture risk calculators assess the risk of fracture based upon several criteria, including age, smoking, alcohol usage, weight, and gender. Osteoporosis is a part of frailty syndrome.
Recently, a study was published by The Journal of Bone and Mineral Research, conducted by researchers from the Tel Aviv University and Hebrew University. This study showed that cannabidiol (CBD) strengthens bones and accelerates the healing of fractures, without causing any psychotropic effects.
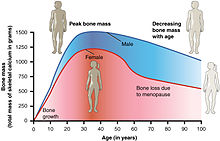
Bone density peaks at about 30 years of age. Women lose bone mass more rapidly than men
Dr. Gorter: “This study proved that CBD alone improves the healing of fractures in all ages and in addition, in the elderly and women in their menopause, prevents or significantly improves osteoporosis (bone loss at older age).”
The team of experts inflicted femoral fractures on rats, and then gave CBD to some of them, while others received CBD plus tetrahydrocannabinol (THC). The conclusion was that, compared to the placebo group, rats fed with CBD alone experienced the same effects, regardless of the addition of THC.
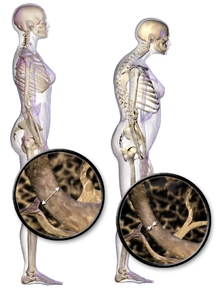
Illustration depicting normal standing posture and in osteoporosis
Dr. Gorter adds: “Clinical observational studies in humans have already proven the benefits of CBD in anti-aging and the prevention of osteoporosis.”
Dr. Gorter: “The same team at the University of Tel-Aviv previously found that the body contains receptors which respond to cannabinoid compounds, and they are not confined to the brain. This study showed that the skeleton has cannabinoid receptors as well which trigger bone formation and prevent bone loss; and the second study just confirmed this.”
and:
“This study is just a part of all research dedicated to the medical benefits of marijuana compounds, and new findings might stimulate researchers to analyze the positive effects of marijuana in the treatment of osteoporosis or other bone diseases.”
The medical properties of Cannabis sativa are numerous, and it is primarily used to boost appetite in the case of AIDS, to lower the side-effects of chemotherapy, and to soothe chronic pain. Numerous studies claim that it can regulate blood sugar, decelerate HIV progression, and treat multiple sclerosis, Parkinson’s disease and various forms of epilepsy.
Dr. Gorter: CBD is a strong COX-1 and COX-2 inhibitor without any side effects. Therefore, CBD inhibits the metastasis of many (all?) cancers and destroys leukemia and lymphoma cells of various kinds.
The journal Neuropsychopharmacology published a 2013 study which discovered that CBD is as effective as several antipsychotic drugs, which are commonly used in the treatment of schizophrenia and paranoia but CBD causes no side-effects. Several studies have also found and confirmed that CBD can be used as a safe antipsychotic.
Dr. Gorter: “We only respond to Cannabis because through evolution, we have developed intrinsic compounds (the so-called Endocannabinoids) and specific receptors that are also activated by compounds in the cannabis plant. One can compare the Endocannabinoid system with the endorphin system and its specific receptors.”
Sources:
http://www.scienceworldreport.com
http://www.business-standard.com
http://www.dnaindia.com
http://www.huffingtonpost.com
http://www.timesofisrael.com
- Jones, Daniel (2003) [1917], Peter Roach, James Hartmann and Jane Setter, eds., English Pronouncing Dictionary, Cambridge: Cambridge University Press, ISBN 3-12-539683-2
- “Osteoporosis”. Merriam-Webster Dictionary.
- “Handout on Health: Osteoporosis”. August 2014. Archivedfrom the original on 18 May 2015. Retrieved 16 May 2015.
- WHO Scientific Group on the Prevention and Management of Osteoporosis (2000 : Geneva, Switzerland) (2003). “Prevention and management of osteoporosis : report of a WHO scientific group”(PDF). pp. 7, 31. ISBN 9241209216. Archived (PDF) from the original on 16 July 2007.
- ^ Jump up to:ab c d e Wells, GA; Cranney, A; Peterson, J; Boucher, M; Shea, B; Robinson, V; Coyle, D; Tugwell, P (23 January 2008). “Alendronate for the primary and secondary prevention of osteoporotic fractures in postmenopausal women”. The Cochrane Database of Systematic Reviews (1): CD001155. doi:10.1002/14651858.CD001155.pub2. PMID 18253985.
- ^ Jump up to:ab c d e Wells, G; Cranney, A; Peterson, J; Boucher, M; Shea, B; Robinson, V; Coyle, D; Tugwell, P (23 January 2008). “Risedronate for the primary and secondary prevention of osteoporotic fractures in postmenopausal women”. The Cochrane Database of Systematic Reviews (1): CD004523. doi:10.1002/14651858.CD004523.pub3. PMID 18254053.
- ^ Jump up to:ab c “Chronic rheumatic conditions”. World Health Organization. Archived from the original on 27 April 2015. Retrieved 18 May 2015.
- Jump up^Golob, AL; Laya, MB (May 2015). “Osteoporosis: Screening, Prevention, and Management”. The Medical clinics of North America. 99 (3): 587–606. doi:10.1016/j.mcna.2015.01.010. PMID 25841602.
- ^ Jump up to:ab Wells GA, Cranney A, Peterson J, Boucher M, Shea B, Robinson V, Coyle D, Tugwell P (23 January 2008). “Etidronate for the primary and secondary prevention of osteoporotic fractures in postmenopausal women”. Cochrane Database of Systematic Reviews (1): CD003376. doi:10.1002/14651858.CD003376.pub3. PMID 18254018.
- Jump up^Nelson HD, Haney EM, Chou R, Dana T, Fu R, Bougatsos C (2010). “Screening for Osteoporosis: Systematic Review to Update the 2002 U.S. Preventive Services Task Force Recommendation [Internet].”. Agency for Healthcare Research and Quality. PMID20722176.
- ^ Jump up to:abc d Wade, SW; Strader, C; Fitzpatrick, LA; Anthony, MS; O’Malley, CD (2014). “Estimating prevalence of osteoporosis: examples from industrialized countries”. Archives of osteoporosis. 9 (1): 182. doi:10.1007/s11657-014-0182-3. PMID 24847682.
- ^ Jump up to:abHanda, R; Ali Kalla, A; Maalouf, G (August 2008). “Osteoporosis in developing countries”. Best practice & research. Clinical rheumatology. 22 (4): 693–708. doi:10.1016/j.berh.2008.04.002. PMID 18783745.
- ^ Jump up to:abSvedbom, A; Hernlund, E; Ivergård, M; Compston, J; Cooper, C; Stenmark, J; McCloskey, EV; Jönsson, B; Kanis, JA; EU Review Panel of, IOF (2013). “Osteoporosis in the European Union: a compendium of country-specific reports”. Archives of osteoporosis. 8 (1–2): 137. doi:10.1007/s11657-013-0137-0. PMC 3880492 . PMID 24113838.
- ^ Jump up to:abWillson, T; Nelson, SD; Newbold, J; Nelson, RE; LaFleur, J (2015). “The clinical epidemiology of male osteoporosis: a review of the recent literature”. Clinical epidemiology. 7: 65–76. doi:10.2147/CLEP.S40966. PMC 4295898 . PMID 25657593.
- Jump up^King, Tekoa L.; Brucker, Mary C. (2011). Pharmacology for women’s health. Sudbury, Mass.: Jones and Bartlett Publishers. p. 1004. ISBN9780763753290. Archived from the original on 8 September 2017.
- Jump up^Old JL, Calvert M (2004). “Vertebral compression fractures in the elderly”. American Family Physician. 69(1): 111–16. PMID 14727827. Archived from the original on 5 August 2011. Retrieved 31 March 2011.
- Jump up^Kim DH, Vaccaro AR (2006). “Osteoporotic compression fractures of the spine; current options and considerations for treatment”. The Spine Journal. 6(5): 479–87. doi:10.1016/j.spinee.2006.04.013. PMID 16934715.
- Jump up^Susan Ott. “Fracture Risk Calculator”. Archivedfrom the original on 14 October 2009. Retrieved 2009-11-03.
- ^ Jump up to:abc WHO (1994). “Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO Study Group”. World Health Organization technical report series. 843: 1–129. PMID 7941614.
- Jump up^Ganz DA, Bao Y, Shekelle PG, Rubenstein LZ (2007). “Will my patient fall?”. JAMA. 297(1): 77–86. doi:10.1001/jama.297.1.77. PMID 17200478.
- Jump up^Waugh EJ, Lam MA, Hawker GA, McGowan J, Papaioannou A, Cheung AM, Hodsman AB, Leslie WD, Siminoski K, Jamal SA (January 2009). “Risk factors for low bone mass in healthy 40–60 year old women: a systematic review of the literature”. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA. 20(1): 1–21. doi:10.1007/s00198-008-0643-x. PMC 5110317 . PMID 18523710.
- Jump up^“6.6 Exercise, Nutrition, Hormones, and Bone Tissue”. Anatomy & Physiology. Openstax CNX. ISBN978-1-938168-13-0. Archived from the original on 10 January 2017.
- Jump up^Sinnesael M, Claessens F, Boonen S, Vanderschueren D (2013). “Novel insights in the regulation and mechanism of androgen action on bone”. Current Opinion in Endocrinology, Diabetes and Obesity. 20(3): 240–44. doi:10.1097/MED.0b013e32835f7d04. PMID 23449008.
- Jump up^Sinnesael M, Boonen S, Claessens F, Gielen E, Vanderschueren D (2011). “Testosterone and the male skeleton: a dual mode of action”. Journal of Osteoporosis. 2011: 240328. doi:10.4061/2011/240328. PMC3173882 . PMID 21941679.
- Jump up^Melton LJ (2003). “Epidemiology worldwide”. Endocrinol. Metab. Clin. North Am. 32(1): v, 1–13. doi:10.1016/S0889-8529(02)00061-0. PMID 12699289.
- ^ Jump up to:abc d e Raisz L (2005). “Pathogenesis of osteoporosis: concepts, conflicts, and prospects”. J Clin Invest. 115 (12): 3318–25. doi:10.1172/JCI27071. PMC 1297264 . PMID 16322775. Archived from the original on 24 August 2007.
- Jump up^Ojo F, Al Snih S, Ray LA, Raji MA, Markides KS (2007). “History of fractures as predictor of subsequent hip and nonhip fractures among older Mexican Americans”. Journal of the National Medical Association. 99(4): 412–18. PMC 2569658 . PMID 17444431.
- ^ Jump up to:abBrian K Alldredge; Koda-Kimble, Mary Anne; Young, Lloyd Y.; Wayne A Kradjan; B. Joseph Guglielmo (2009). Applied therapeutics: the clinical use of drugs. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins. pp. 101–03. ISBN 0-7817-6555-2.
- ^ Jump up to:abPoole KE, Compston JE (December 2006). “Osteoporosis and its management”. BMJ. 333 (7581): 1251–56. doi:10.1136/bmj.39050.597350.47. PMC 1702459 . PMID 17170416.
- Jump up^Berg KM, Kunins HV, Jackson JL, Nahvi S, Chaudhry A, Harris KA, Malik R, Arnsten JH (2008). “Association between alcohol consumption and both osteoporotic fracture and bone density”. Am J Med. 121(5): 406–18. doi:10.1016/j.amjmed.2007.12.012. PMC 2692368 . PMID 18456037.
- Jump up^Nieves JW (2005). “Osteoporosis: the role of micronutrients”. Am J Clin Nutr. 81(5): 1232S–39S. doi:10.1093/ajcn/81.5.1232. PMID 15883457. Archivedfrom the original on 24 April 2008.
- Jump up^Gielen E, Boonen S, Vanderschueren D, Sinnesael M, Verstuyf A, Claessens F, Milisen K, Verschueren S (2011). “Calcium and vitamin d supplementation in men”. Journal of Osteoporosis. 2011: 875249. doi:10.4061/2011/875249. PMC3163142 . PMID 21876835.
- Jump up^Wong PK, Christie JJ, Wark JD (2007). “The effects of smoking on bone health”. Clin. Sci. 113(5): 233–41. doi:10.1042/CS20060173. PMID 17663660.
- Jump up^Ilich JZ, Kerstetter JE (2000). “Nutrition in Bone Health Revisited: A Story Beyond Calcium”. Journal of the American College of Nutrition. 19(6): 715–37. doi:10.1080/07315724.2000.10718070. PMID 11194525. Archived from the original on 7 August 2009.
- Jump up^Weiss LA, Barrett-Connor E, von Mühlen D (2005). “Ratio of n−6 to n−3 fatty acids and bone mineral density in older adults: the Rancho Bernardo Study”. Am J Clin Nutr April. 81(4): 934–38. doi:10.1093/ajcn/81.4.934. PMID 15817874. Archivedfrom the original on 24 October 2009.
- Jump up^Abelow BJ, Holford TR, Insogna KL (1992). “Cross-cultural association between dietary animal protein and hip fracture: a hypothesis”. Calcified tissue international. 50(1): 14–18. doi:10.1007/BF00297291. PMID 1739864.
- Jump up^Hegsted M, Schuette SA, Zemel MB, Linkswiler HM (1981). “Urinary calcium and calcium balance in young men as affected by level of protein and phosphorus intake”. The Journal of Nutrition. 111(3): 553–62. doi:10.1093/jn/111.3.553. PMID 7205408.
- Jump up^Kerstetter JE, Allen LH (1990). “Dietary protein increases urinary calcium”(PDF). Journal of Nutrition. 120 (1): 134–36. doi:10.1093/jn/120.1.134. PMID 2406396.
- Jump up^Feskanich D, Willett WC, Stampfer MJ, Colditz GA (1996). “Protein consumption and bone fractures in women”. Am. J. Epidemiol. 143(5): 472–79. doi:10.1093/oxfordjournals.aje.a008767. PMID 8610662.
- Jump up^Kerstetter JE, Kenny AM, Insogna KL (2011). “Dietary protein and skeletal health: A review of recent human research”. Current Opinion in Lipidology. 22(1): 16–20. doi:10.1097/MOL.0b013e3283419441. PMC 4659357 . PMID 21102327.
- Jump up^Bonjour JP (2005). “Dietary protein: An essential nutrient for bone health”. Journal of the American College of Nutrition. 24(6 Suppl): 526S–36S. doi:10.1080/07315724.2005.10719501. PMID 16373952.
- Jump up^Kerstetter JE, O’Brien KO, Insogna KL (2003). “Dietary protein, calcium metabolism, and skeletal homeostasis revisited”. Am. J. Clin. Nutr. 78(3 Suppl): 584S–92S. PMID 12936953.
- Jump up^Schönau E, Werhahn E, Schiedermaier U, Mokow E, Schiessl H, Scheidhauer K, Michalk D (1996). “Influence of muscle strength on bone strength during childhood and adolescence”. Hormone Research. 45(Suppl. 1): 63–66. doi:10.1159/000184834. PMID 8805035.
- Jump up^Shapses SA, Riedt CS (1 June 2006). “Bone, body weight, and weight reduction: what are the concerns?”. J. Nutr. 136(6): 1453–56. doi:10.1093/jn/136.6.1453. PMC 4016235 . PMID 16702302. Archived from the original on 10 March 2008.
- Jump up^Pollock N, Grogan C, Perry M, Pedlar C, Cooke K, Morrissey D, Dimitriou L (2010). “Bone-mineral density and other features of the female athlete triad in elite endurance runners: A longitudinal and cross-sectional observational study”. International journal of sport nutrition and exercise metabolism. 20(5): 418–26. doi:10.1123/ijsnem.20.5.418. PMID 20975110.
- Jump up^Gibson JH, Mitchell A, Harries MG, Reeve J (2004). “Nutritional and exercise-related determinants of bone density in elite female runners”. Osteoporosis International. 15(8): 611–18. doi:10.1007/s00198-004-1589-2. PMID 15048548.
- Jump up^Hetland ML, Haarbo J, Christiansen C (1993). “Low bone mass and high bone turnover in male long distance runners”. The Journal of Clinical Endocrinology and Metabolism. 77(3): 770–75. doi:10.1210/jcem.77.3.8370698. PMID 8370698.
- Jump up^Brahm H, Ström H, Piehl-Aulin K, Mallmin H, Ljunghall S (1997). “Bone metabolism in endurance trained athletes: A comparison to population-based controls based on DXA, SXA, quantitative ultrasound, and biochemical markers”. Calcified tissue international. 61(6): 448–54. doi:10.1007/s002239900366. PMID 9383270.
- Jump up^MacKelvie KJ, Taunton JE, McKay HA, Khan KM (2000). “Bone mineral density and serum testosterone in chronically trained, high mileage 40–55 year old male runners”. British journal of sports medicine. 34(4): 273–78. doi:10.1136/bjsm.34.4.273. PMC 1724199 . PMID 10953900.
- Jump up^Staessen JA, Roels HA, Emelianov D, Kuznetsova T, Thijs L, Vangronsveld J, Fagard R (1999). “Environmental exposure to cadmium, forearm bone density, and risk of fractures: prospective population study. Public Health and Environmental Exposure to Cadmium (PheeCad) Study Group”. Lancet. 353(9159): 1140–44. doi:10.1016/S0140-6736(98)09356-8. PMID 10209978.
- Jump up^Tucker KL, Morita K, Qiao N, Hannan MT, Cupples LA, Kiel DP (2006). “Colas, but not other carbonated beverages, are associated with low bone mineral density in older women: The Framingham Osteoporosis Study”. Am. J. Clin. Nutr. 84(4): 936–42. PMID 17023723.
- Jump up^American Academy of Pediatrics Committee on School Health (2004). “Soft drinks in schools”. Pediatrics. 113(1 Pt 1): 152–54. doi:10.1542/peds.113.1.152. PMID 14702469.
- Jump up^Zhou, B.; Huang, Y.; Li, H.; Sun, W.; Liu, J. (13 October 2015). “Proton-pump inhibitors and risk of fractures: an update meta-analysis”. Osteoporosis International. 27(1): 339–47. doi:10.1007/s00198-015-3365-x. PMID 26462494.
- ^ Jump up to:abc d e Simonelli, C; et al. (July 2006). “ICSI Health Care Guideline: Diagnosis and Treatment of Osteoporosis, 5th edition”. Institute for Clinical Systems Improvement. Archived from the original (PDF) on 18 July 2007. Retrieved 2008-04-08.
- ^ Jump up to:abc d e f g h i j k l Kohlmeier, Lynn Kohlmeier (1998). “Osteoporosis – Risk Factors, Screening, and Treatment”. Medscape Portals. Archived from the original on 19 December 2008. Retrieved 2008-05-11.
- ^ Jump up to:abc Ebeling PR (2008). “Clinical practice. Osteoporosis in men”. N Engl J Med. 358 (14): 1474–82. doi:10.1056/NEJMcp0707217. PMID 18385499.
- ^ Jump up to:abMirza F, Canalis E (Sep 2015). “Management of endocrine disease: Secondary osteoporosis: pathophysiology and management”. Eur J Endocrinol (Review). 173 (3): R131–51. doi:10.1530/EJE-15-0118. PMC 4534332 . PMID 25971649. Archived from the original on 16 February 2016.
- ^ Jump up to:abc Henwood MJ, Binkovitz L (2009). “Update on pediatric bone health”. The Journal of the American Osteopathic Association. 109 (1): 5–12. PMID 19193819. Archived from the original on 4 March 2016.
- Jump up^Beto JA (Jan 2015). “The role of calcium in human aging”. Clin Nutr Res (Review). 4(1): 1–8. doi:10.7762/cnr.2015.4.1.1. PMC 4337919 . PMID 25713787.
- Jump up^Mornet, PhD, Etienne; Nunes, MD, Mark E (20 November 2007). GeneReviews: Hypophostasia. NCBI. Archivedfrom the original on 18 January 2017.
- Jump up^“Hypophosphatasia Case Studies: Dangers of Misdiagnosis”. Hypophosphatasia.com. Archivedfrom the original on 8 August 2014. Retrieved 5 August 2014.
- Jump up^Invernizzi M, Carda S, Viscontini GS, Cisari C (2009). “Osteoporosis in Parkinson’s disease”. Parkinsonism & Related Disorders. 15(5): 339–46. doi:10.1016/j.parkreldis.2009.02.009. PMID 19346153.
- Jump up^Celsi F, Pizzo P, Brini M, Leo S, Fotino C, Pinton P, Rizzuto R (2009). “Mitochondria, calcium and cell death: A deadly triad in neurodegeneration”. Biochimica et Biophysica Acta (BBA) – Bioenergetics. 1787(5): 335–44. doi:10.1016/j.bbabio.2009.02.021. PMC 2696196 . PMID 19268425.
- Jump up^Bone and Tooth Society of Great Britain, National Osteoporosis Society, Royal College of Physicians (2003). Glucocorticoid-induced Osteoporosis(PDF). London, UK: Royal College of Physicians of London. ISBN 1-86016-173-1. Archived (PDF) from the original on 14 January 2012.
- Jump up^Gourlay M, Franceschini N, Sheyn Y (2007). “Prevention and treatment strategies for glucocorticoid-induced osteoporotic fractures”. Clin Rheumatol. 26(2): 144–53. doi:10.1007/s10067-006-0315-1. PMID 16670825.
- Jump up^Petty SJ, O’Brien TJ, Wark JD (2007). “Anti-epileptic medication and bone health”. Osteoporosis international. 18(2): 129–42. doi:10.1007/s00198-006-0185-z. PMID 17091219.
- Jump up^Ruiz-Irastorza G, Khamashta MA, Hughes GR (2002). “Heparin and osteoporosis during pregnancy: 2002 update”. Lupus. 11(10): 680–82. doi:10.1191/0961203302lu262oa. PMID 12413068.
- Jump up^Gage BF, Birman-Deych E, Radford MJ, Nilasena DS, Binder EF (2006). “Risk of osteoporotic fracture in elderly patients taking warfarin: results from the National Registry of Atrial Fibrillation 2”. Arch. Intern. Med. 166(2): 241–46. doi:10.1001/archinte.166.2.241. PMID 16432096. Archived from the original on 23 March 2012.
- Jump up^Yang YX, Lewis JD, Epstein S, Metz DC (2006). “Long-term proton pump inhibitor therapy and risk of hip fracture”. JAMA. 296(24): 2947–53. doi:10.1001/jama.296.24.2947. PMID 17190895.
- Jump up^Murphy CE, Rodgers PT (2007). “Effects of thiazolidinediones on bone loss and fracture”. Annals of Pharmacotherapy. 41(12): 2014–18. doi:10.1345/aph.1K286. PMID 17940125.
- ^ Jump up to:abLatimer B (2005). “The perils of being bipedal”. Ann Biomed Eng. 33 (1): 3–6. doi:10.1007/s10439-005-8957-8. PMID 15709701.
- ^ Jump up to:abc Cotter M et. al (2011). “Human evolution and osteoporosis-related spinal fractures”. PLoS ONE. 6 (10): e26658. Bibcode:2011PLoSO…626658C. doi:10.1371/journal.pone.0026658. PMC 3197574 . PMID 22028933.
- Jump up^Eaton SB, Nelson DA (1991). “Calcium in evolutionary perspective”. Am. J. Clin. Nutr. 54(1 Suppl): 281S–87S. PMID 2053574.
- Jump up^Frost HM, Thomas CC. Bone Remodeling Dynamics. Springfield, IL: 1963.
- Jump up^Wu, Shuyan (2013). “Genome-wide approaches for identifying genetic risk factors for osteoporosis”. Genome Med. 5(5): 44. doi:10.1186/gm448. PMC 3706967 . PMID 23731620. Archived from the original on 27 April 2015.
- Jump up^Paccou, Julien; Hardouin, Pierre; Cotten, Anne; Penel, Guillaume; Cortet, Bernard (1 October 2015). “The Role of Bone Marrow Fat in Skeletal Health: Usefulness and Perspectives for Clinicians”. The Journal of Clinical Endocrinology & Metabolism. 100(10): 3613–21. doi:10.1210/jc.2015-2338. ISSN 0021-972X.
- ^ Jump up to:abc Guglielmi G, Scalzo G (6 May 2010). “Imaging tools transform diagnosis of osteoporosis”. Diagnostic Imaging Europe. 26: 7–11. Archived from the original on 2 June 2010.
- Jump up^Leib ES, Lewiecki EM, Binkley N, Hamdy RC (2004). “Official positions of the International Society for Clinical Densitometry”. J Clin Densitom. 7(1): 1–5. doi:10.1385/JCD:7:1:1. PMID 14742881. quoted in: “Diagnosis of osteoporosis in men, premenopausal women, and children” Archived 24 February 2008 at the Wayback Machine.
- Jump up^Yasuda Y, Kaleta J, Brömme D (2005). “The role of cathepsins in osteoporosis and arthritis: rationale for the design of new therapeutics”. Adv. Drug Deliv. Rev. 57(7): 973–93. doi:10.1016/j.addr.2004.12.013. PMID 15876399.
- Jump up^Meunier, Pierre (1998). Osteoporosis: Diagnosis and Management. London: Taylor and Francis. ISBN1-85317-412-2.
- Jump up^Bindex, a Radiation-Free Device for Osteoporosis Screening, FDA Cleared. May 2016Archived 15 June 2016 at the Wayback Machine.
- ^ Jump up to:abc d U.S. Preventive Services Task, Force (1 March 2011). “Screening for osteoporosis: U.S. preventive services task force recommendation statement”. Annals of Internal Medicine. 154 (5): 356–64. doi:10.7326/0003-4819-154-5-201103010-00307. PMID 21242341.
- Jump up^“100 most recent Archives 2017 2016 2015 2014 2013 2012 2011 2010 2009 2008 2007 2006 2005 Bone fragility: preventing fractures”. Prescrire International. 26(181): 103–06. April 2017. Archived from the original on 8 September 2017.
- Jump up^International Society for Clinical Densitometry (ISCD). 2013 ISCD Official Positions – Adult. (2013). at “Archived copy”. Archivedfrom the original on 5 May 2015. Retrieved 2015-05-04.
- Jump up^Rud B, Hilden J, Hyldstrup L, Hróbjartsson A (2009). “The Osteoporosis Self-Assessment Tool versus alternative tests for selecting postmenopausal women for bone mineral density assessment: a comparative systematic review of accuracy”. Osteoporos Int. 20(4): 599–607. doi:10.1007/s00198-008-0713-0. PMID 18716823.
- Jump up^Ebeling, PR.; Daly, RM.; Kerr, DA.; Kimlin, MG. (Oct 2013). “Building healthy bones throughout life: an evidence-informed strategy to prevent osteoporosis in Australia”. Med J Aust. 199(7 Suppl): S1. hdl:10536/DRO/DU:30060407. PMID 25370432.
- ^ Jump up to:abc d e f g h i Body JJ (2011). “How to manage postmenopausal osteoporosis?”. Acta Clin Belg. 66 (6): 443–47. doi:10.1179/ACB.66.6.2062612. PMID 22338309.
- ^ Jump up to:abLudvigsson JF, Bai JC, Biagi F, Card TR, Ciacci C, Ciclitira PJ, Green PH, Hadjivassiliou M, Holdoway A, van Heel DA, Kaukinen K, Leffler DA, Leonard JN, Lundin KE, McGough N, Davidson M, Murray JA, Swift GL, Walker MM, Zingone F, Sanders DS; BSG Coeliac Disease Guidelines Development Group; British Society of Gastroenterology (Aug 2014). “Diagnosis and management of adult coeliac disease: guidelines from the British Society of Gastroenterology”. Gut (Review). 63 (8): 1210–28. doi:10.1136/gutjnl-2013-306578. PMC 4112432 . PMID 24917550.
- Jump up^“Drugs for Postmenopausal Osteoporosis”. The Medical Letter on Drugs and Therapeutics. 56(1452): 91–96. 29 September 2014.
- ^ Jump up to:abc d Moyer, VA; on behalf of the U.S. Preventive Services Task, Force (26 Feb 2013). “Vitamin D and Calcium Supplementation to Prevent Fractures in Adults: U.S. Preventive Services Task Force Recommendation Statement”. Annals of Internal Medicine. 158 (9): 691–96. doi:10.7326/0003-4819-158-9-201305070-00603. PMID 23440163.
- Jump up^Bolland, MJ; Leung, W; Tai, V; Bastin, S; Gamble, GD; Grey, A; Reid, IR (29 September 2015). “Calcium intake and risk of fracture: systematic review”. BMJ (Clinical research ed.). 351: h4580. doi:10.1136/bmj.h4580. PMC4784799 . PMID 26420387.
- Jump up^DIPART (vitamin D Individual Patient Analysis of Randomized Trials) (2010). “Patient level pooled analysis of 68 500 patients from seven major vitamin D fracture trials in US and Europe”. BMJ. 340: b5463. doi:10.1136/bmj.b5463. PMC2806633 . PMID 20068257.
- ^ Jump up to:abc Avenell, A; Mak, JC; O’Connell, D (14 April 2014). “Vitamin D and vitamin D analogues for preventing fractures in post-menopausal women and older men”. The Cochrane Database of Systematic Reviews. 4 (4): CD000227. doi:10.1002/14651858.CD000227.pub4. PMID 24729336.
- Jump up^Bolland MJ, Avenell A, Baron JA, Grey A, MacLennan GS, Gamble GD, Reid IR (2010). “Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: meta-analysis”. BMJ (Clinical research ed.). 341: c3691. doi:10.1136/bmj.c3691. PMC2912459 . PMID 20671013.
- Jump up^Bolland MJ, Grey A, Avenell A, Gamble GD, Reid IR (2011). “Calcium supplements with or without vitamin D and risk of cardiovascular events: reanalysis of the Women’s Health Initiative limited access dataset and meta-analysis”. BMJ. 342: d2040. doi:10.1136/bmj.d2040. PMC3079822 . PMID 21505219.
- Jump up^Hosoi, T (2010). “Genetic aspects of osteoporosis”. Journal of Bone and Mineral Metabolism. 28(6): 601–07. doi:10.1007/s00774-010-0217-9.
- Jump up^Cockayne S, Adamson J, Lanham-New S, Shearer MJ, Gilbody S, Torgerson DJ (2006). “Vitamin K and the Prevention of Fractures: Systematic Review and Meta-analysis of Randomized Controlled Trials”. Archives of Internal Medicine. 166(12): 1256–61. doi:10.1001/archinte.166.12.1256. PMID 16801507.
- Jump up^Iwamoto J, Sato Y (2013). “Menatetrenone for the treatment of osteoporosis”. Expert Opin Pharmacother. 14(4): 449–58. doi:10.1517/14656566.2013.763796. PMID 23346882.
- ^ Jump up to:abc d e Howe TE, Shea B, Dawson LJ, Downie F, Murray A, Ross C, Harbour RT, Caldwell LM, Creed G (2011). “Exercise for preventing and treating osteoporosis in postmenopausal women”. Cochrane Database of Systematic Reviews. Art. No.: CD000333 (7). doi:10.1002/14651858.CD000333.pub2 – via Cochrane Database of Systematic Reviews.
- Jump up^Body JJ, Bergmann P, Boonen S, Boutsen Y, Bruyere O, Devogelaer JP, Goemaere S, Hollevoet N, Kaufman JM, Milisen K, Rozenberg S, Reginster JY (2011). “Non-pharmacological management of osteoporosis: a consensus of the Belgian Bone Club”. Osteoporos Int. 22 (11): 2769–88. doi:10.1007/s00198-011-1545-x. PMC 3186889 . PMID 21360219.
- Jump up^Kasturi GC, Adler RA (2011). “Osteoporosis: nonpharmacologic management”. PM&R. 3 (6): 562–72. doi:10.1016/j.pmrj.2010.12.014. PMID 21478069.
- ^ Jump up to:ab Whitaker M, Guo J, Kehoe T, Benson G (2012). “Bisphosphonates for osteoporosis – where do we go from here?”. N. Engl. J. Med. 366 (22): 2048–51. doi:10.1056/NEJMp1202619. PMID 22571168.
- Jump up^Suresh E, Pazianas M, Abrahamsen B (Jan 2014). “Safety issues with bisphosphonate therapy for osteoporosis”. Rheumatology (Oxford, England). 53 (1): 19–31. doi:10.1093/rheumatology/ket236. PMID 23838024.
- ^ Jump up to:ab Adler, Robert A; El-Hajj Fuleihan, Ghada; Bauer, Douglas C; Camacho, Pauline M; Clarke, Bart L; Clines, Gregory A; Compston, Juliet E; Drake, Matthew T; Edwards, Beatrice J; Favus, Murray J; Greenspan, Susan L; McKinney, Ross; Pignolo, Robert J; Sellmeyer, Deborah E (January 2016). “Managing Osteoporosis in Patients on Long-Term Bisphosphonate Treatment: Report of a Task Force of the American Society for Bone and Mineral Research”. Journal of Bone and Mineral Research. 31 (1): 16–35. doi:10.1002/jbmr.2708. PMC 4906542 . PMID 26350171.
- ^ Jump up to:ab c Qaseem, Amir; Forciea, Mary Ann; McLean, Robert M.; Denberg, Thomas D. (9 May 2017). “Treatment of Low Bone Density or Osteoporosis to Prevent Fractures in Men and Women: A Clinical Practice Guideline Update from the American College of Physicians”. Annals of Internal Medicine. 166 (11): 818–39. doi:10.7326/M15-1361. PMID 28492856.
- Jump up^Davis S, Sachdeva A, Goeckeritz B, Oliver A (2010). “Approved treatments for osteoporosis and what’s in the pipeline”. Drug Benefit Trends. 22 (4): 121–24. Archived from the original on 28 July 2010.
- ^ Jump up to:ab Nayak, S; Greenspan, SL (March 2017). “Osteoporosis Treatment Efficacy for Men: A Systematic Review and Meta-Analysis”. Journal of the American Geriatrics Society. 65 (3): 490–95. doi:10.1111/jgs.14668. PMC 5358515 . PMID 28304090.
- Jump up^Haguenauer, D; Welch, V; Shea, B; Tugwell, P; Wells, G (2000). “Fluoride for treating postmenopausal osteoporosis”. The Cochrane Database of Systematic Reviews (4): CD002825. doi:10.1002/14651858.CD002825. PMID 11034769.
- Jump up^Vestergaard, P; Jorgensen, NR; Schwarz, P; Mosekilde, L (March 2008). “Effects of treatment with fluoride on bone mineral density and fracture risk – a meta-analysis”. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA. 19 (3): 257–68. doi:10.1007/s00198-007-0437-6. PMID 17701094.
- Jump up^Han SL, Wan SL (February 2012). “Effect of teriparatide on bone mineral density and fracture in postmenopausal osteoporosis: meta-analysis of randomised controlled trials”. International journal of clinical practice. 66 (2): 199–209. doi:10.1111/j.1742-1241.2011.02837.x. PMID 22257045.
- Jump up^O’Donnell, S.; Cranney, A.; Wells, G. A.; Adachi, J. D.; Reginster, J. Y. (18 October 2006). “Strontium ranelate for preventing and treating postmenopausal osteoporosis”. The Cochrane Database of Systematic Reviews (4): CD005326. doi:10.1002/14651858.CD005326.pub3. ISSN 1469-493X. PMID 17054253.
- Jump up^“Background Document for Meeting of Advisory Committee for Reproductive Health Drugs and Drug Safety and Risk Management Advisory Committee” (PDF). FDA. Mar 2013. Archived (PDF) from the original on 9 June 2013.
- Jump up^“Osteoporosis – primary prevention (TA160) : Alendronate, etidronate, risedronate, raloxifene and strontium ranelate for the primary prevention of osteoporotic fragility fractures in postmenopausal women”. UK: National Institute for Health and Care Excellence (NICE). January 2011. Archived from the original on 22 October 2013.
- Jump up^Cranney A, Jamal SA, Tsang JF, Josse RG, Leslie WD (2007). “Low bone mineral density and fracture burden in postmenopausal women”. CMAJ. 177 (6): 575–80. doi:10.1503/cmaj.070234. PMC 1963365 . PMID 17846439.
- Jump up^Hannan EL, Magaziner J, Wang JJ, Eastwood EA, Silberzweig SB, Gilbert M, Morrison RS, McLaughlin MA, Orosz GM, Siu AL (2001). “Mortality and locomotion 6 months after hospitalization for hip fracture: risk factors and risk-adjusted hospital outcomes”. JAMA. 285 (21): 2736–42. doi:10.1001/jama.285.21.2736. PMID 11386929.
- Jump up^Brenneman SK, Barrett-Connor E, Sajjan S, Markson LE, Siris ES (2006). “Impact of recent fracture on health-related quality of life in postmenopausal women”. J. Bone Miner. Res. 21 (6): 809–16. doi:10.1359/jbmr.060301. PMID 16753011.
- ^ Jump up to:ab Riggs BL, Melton LJ (1995). “The worldwide problem of osteoporosis: insights afforded by epidemiology”. Bone. 17 (5 Suppl): 505S–11S. doi:10.1016/8756-3282(95)00258-4. PMID 8573428.
- ^ Jump up to:ab “MerckMedicus Modules: Osteoporosis – Epidemiology”. Merck & Co., Inc. Archived from the original on 28 December 2007. Retrieved 2008-06-13.
- Jump up^Cauley JA, Hochberg MC, Lui LY, Palermo L, Ensrud KE, Hillier TA, Nevitt MC, Cummings SR (2007). “Long-term risk of incident vertebral fractures”. JAMA. 298 (23): 2761–67. doi:10.1001/jama.298.23.2761. PMID 18165669.
- Jump up^International Osteoporosis Foundation. EpidemiologyArchived 9 August 2015 at the Wayback Machine..
- ^ Jump up to:ab c “The Global Burden of Osteoporosis | International Osteoporosis Foundation”. www.iofbonehealth.org. Archivedfrom the original on 5 March 2016. Retrieved 2016-02-09.
- ^ Jump up to:ab c Cauley, Jane A. (23 March 2011). “Defining Ethnic and Racial Differences in Osteoporosis and Fragility Fractures”. Clinical Orthopaedics and Related Research®. 469 (7): 1891–99. doi:10.1007/s11999-011-1863-5. ISSN 0009-921X. PMC 3111798 . PMID 21431462.
- ^ Jump up to:ab Kanis, J. A.; Odén, A.; McCloskey, E. V.; Johansson, H.; Wahl, D. A.; Cooper, C.; Life, on behalf of the IOF Working Group on Epidemiology and Quality of (15 March 2012). “A systematic review of hip fracture incidence and probability of fracture worldwide”. Osteoporosis International. 23 (9): 2239–56. doi:10.1007/s00198-012-1964-3. ISSN 0937-941X. PMC 3421108 . PMID 22419370.
- Jump up^Herrmann, Markus; Schmidt, Johannes Peter; Umanskaya, Natalia; Wagner, Alexandra; Taban-Shomal, Omid; Widmann, Thomas; Colaianni, Graziana; Wildemann, Britt; Herrmann, Wolfgang (2007). “The role of hyperhomocysteinemia as well as folate, vitamin B6 and B12 deficiencies in osteoporosis – a systematic review”. Clinical Chemical Laboratory Medicine. 45 (12). doi:10.1515/cclm.2007.362.
- Jump up^Gerald N. Grob (2014). Aging Bones: A Short History of Osteoporosis. Johns Hopkins UP. p. 5. ISBN 9781421413181. Archived from the original on 23 July 2014.
- Jump up^Albright F, Bloomberg E, Smith PH (1940). “Postmenopausal osteoporosis”. Trans. Assoc. Am. Physicians. 55: 298–305.
- Jump up^Patlak M (2001). “Bone builders: the discoveries behind preventing and treating osteoporosis”. FASEB J. 15 (10): 1677E. doi:10.1096/fj.15.10.1677e. PMID 11481214.
- Jump up^Hirata, K.; Morimoto, I. (1994). “Vertebral Osteoporosis in Late Edo Japanese”. Anthropological Science. 102 (4): 345–61. doi:10.1537/ase.102.345. Archived from the original on 22 December 2015. Retrieved 18 December 2015.
Hello
I would like to invite you to list robert-gorter.info with LoveToCBD.com, the World’s First CBD Online Shop Marketplace for CBD products.
A Little Bit About Us
LoveToCBD.com is the world’s first ever CBD marketplace aimed at all businesses operating in the CBD industry. Here, you can buy and sell all types of CBD products without leaving our website. LoveToCBD.com effectively brings together ALL types of CBD businesses from all parts of the world. Just think of our platform as a collection of all CBD e-commerce shops and websites offering ALL products and brands under one roof. The platform has already been featured in leading newspapers and magazines and its active CBD blog is growing its subscriber base and site traffic.
Learn more: https://lovetocbd.com/about-us
How it works: https://lovetocbd.com/how-it-works
I look forward to seeing you onboard.
Kind regards